Can I exercise after a heart attack? What kind of exercise should I do? How much exercise? What physical activities are safe? Should I enroll in a cardiac rehab program?
You surely have a lot of questions rattling around your head, so the purpose is to answer them and give you some peace of mind.
A heart attack, shorthand speak for a myocardial infarction or cardiac arrest, is a life-altering event that may lead to significant anxiety which can compromise your quality of life.
If you already participate in regular physical activity, a heart attack can be anxiety provoking and take its toll on your mental health when trying to get back to your normal activities.
In my previous posts on exercise for angioplasty/stent, coronary artery bypass surgery, heart valve surgery, implanted cardioverter defibrillator (ICD), and atrial fibrillation, I lightly touched on heart attacks and how the exercise “playing field” changes after you’ve had one.
But I’d like to assure you that once you’ve had a heart attack, or any other cardiac episode for that matter, your life is NOT over. Pretty far from it.
As a clinical exercise physiologist having worked in cardiac rehabilitation and research settings, I’ve helped a lot of people who’ve had heart attacks and, after receiving professional medical advice, getting proper treatment, and sticking to a robust exercise program, they’ve gone on to live very active and productive lives.
- What is a heart attack?
- Angina vs heart attack: what's the difference?
- Signs and symptoms of angina
- Time is heart muscle: get help fast!
- Risk factors for heart attack
- Cardiac rehabilitation after a heart attack
- Can I exercise after a heart attack?
- When can I exercise after a heart attack?
- Benefits of exercise after a heart attack
- What’s the best exercise after a heart attack?
- Inpatient exercise guidelines
- Outpatient exercise guidelines
- Strength training (resistance training) after a heart attack
- Yoga and Tai Chi
- Take home message
What is a heart attack?
It amazes me that some heart attack patients I’ve worked with had quite large heart attacks but really had no conceptual understanding of exactly what a heart attack is.
And this lack of awareness only served to make them more anxious and afraid to do any physical exercise.
Heart function basics
In the simplest terms, your heart is just a pump that circulates blood throughout the body.
But your heart must ALSO pump oxygen- and nutrient-rich blood to itself which it does through the coronary arteries (see image below).
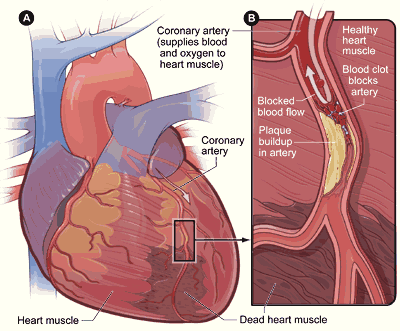
Coronary arteries are a network of blood vessels which wrap around and envelop the heart muscle.
A heart attack, or myocardial infarction (MI), is a medical emergency that occurs when coronary artery disease causes a blockage in the arteries that feed blood to your heart muscle.
The ‘downstream’ heart muscle on the other side of the blockage is starved of oxygen and nutrients and, without immediate medical help, can result in death of the cardiac tissue (muscle) served by the blocked artery.
Timely treatment results in better outcomes, long-term benefits, and a significantly reduced risk of death from a subsequent heart attack. It can also yield a lower risk of developing heart failure and arrhythmias (i.e., abnormal heart rhythms or irregular heartbeat) like atrial fibrillation that can lead to blood clots, a major risk factor for stroke.
Heart attack survivors that are proactive about their heart health work with their medical management team to eat a healthy diet, maintain a lower blood pressure, cholesterol levels, and blood sugar values (if diabetic).
If you’re a visual learner, here is a short clip about heart attacks with 3D animation which succinctly summarises the process.
Angina vs heart attack: what’s the difference?
When a coronary artery has a blockage, chest pain, commonly referred to as angina, is your early warning sign.
But the blockage does not have to be 100%.
In many cases, it is possible to have, for example, a 70% blockage in an artery and have no symptoms whatsoever at rest.
But under exertion from exercise, such as when walking up a hill or some other sort of strenuous aerobic activity, the heart muscle’s demand for blood (and the oxygen and nutrients it carries) is exceeded by the coronary arteries’ ability to supply it.
For most people, this results in the standard tell-tale symptoms like jaw, chest, back, or arm pain, sweating, lightheadedness, dizziness, or other atypical pain (i.e., referred pain to the low back).
The good news is that this is only a plumbing problem in your coronary arteries and NOT a heart attack (though can turn into a heart attack if left unattended).
Often when you stop exercise, the pain will go away.
If the pain is predictably consistent with activity, then it is known as stable angina.
Alternatively, when you’re sitting at home in your chair watching TV and the chest pain kicks in without warning, this is known as unstable angina.
Obviously the latter is more critical, but both situations warrant immediate medical attention.
Signs and symptoms of angina
- Chest pain or discomfort (sometimes mistaken for heart burn)
- Shortness of breath
- Pain radiating down the left arm (or both arms), the back, neck, jaw, or the abdominal area
- Feeling queasy/nauseous, vomiting, cold sweat, dizziness
- Atypical pain which might occur in between the shoulder blades or in the lower back (not common, but I’ve seen it in clinical practice)
A heart attack, on the other hand, occurs when the blood flow through a coronary artery is completely blocked.
This may occur suddenly when a blockage in the artery ruptures and the impending blood clot impedes blood flow.
In other cases, an abnormal cardiac rhythm can cause the heart to stop, but this is not the same as ischemic heart disease (blocked arteries).
For people with underlying cardiac risk factors, such things like shovelling snow or playing a ‘weekend warrior’ game of football can precipitate a heart attack.
Time is heart muscle: get help fast!
The onset of angina is your cue to get to the hospital as soon as possible.
In cardiac rehab, we have a saying which goes “time is heart muscle.”
The quicker they evaluate you, administer clot busting drugs, and/or perform an emergency angioplasty (or bypass surgery), the more likely you are to preserve your heart muscle.
How do you know you’re at risk for a heart attack (or second heart attack)?
Be aware of the following cardiovascular risk factors which may predispose you to heart problems:
Risk factors for heart attack
The American College of Sports Medicine’s Guidelines for Exercise Testing and Prescription is the bible for exercise physiologists and provides excellent information on exercise after a heart attack.
Cardiovascular disease risk factors
Age
Male: 45 years or older; Female: 55 years or older
Family history
Heart attack, coronary artery bypass surgery, or sudden death in an immediate blood relative (before age 55 in male 1st degree relative or before age 65 in female relative)
Cigarette smoking
Current smoker or those who quit within the past 6 months. Click here for information on how cigarettes affect your blood vessels.
High blood pressure
Systolic blood pressure of 140 mmHg or diastolic blood pressure of 90 mmHg or greater confirmed by measurements on at least two separate occasions, or taking prescribed blood pressure medication. This Mayo Clinic article discusses the impact of blood pressure on your heart and body.
Sedentary lifestyle
Not participating in at least 30 minutes of moderate intensity physical activity on at least three days of the week for at least three months
Obesity
Body mass index of 30 kg/m2 or greater or waist measurement of 40 inches or greater (> 102 cm) for men and 35 inches or greater (>88 cm) for women. This article in the cardiologist journal Circulation discusses the link between obesity and heart disease.
High cholesterol
Total cholesterol is 200 mg/dl or greater (5.18 mmol/l); LDL cholesterol is 130 mg/dl or greater (3.37 mmol/l); or HDL is less than 40 mg/dl (1.04 mmol/l)
Pre-diabetes
Glucose levels after an overnight fast are between 100 to 126 mg/dl (5.5 to 6.93 mmol/l) or glucose levels after a 75g oral glucose tolerance test are between 140 to 200 mg/dl (7.7 to 11 mmol/L). There is a strong link between diabetes and cardiovascular risk. If you HAVE diagnosed diabetes, you are at a 2-4 times greater risk of heart attack and stroke. Keep your blood glucose levels under control.
Protective HDL Levels
HDL is your “good” cholesterol which protects you against heart disease. A level of 60 mg/dl (1.55 mmol/l) is desirable
For more information on diet after a heart attack, read Gabby Maston’s article on the paleo diet vs. the Mediterranean diet.
Cardiac rehabilitation after a heart attack
Being a former cardiac rehabilitation exercise physiologist, I admit I’m biased when it comes to recommending cardiac rehab after a heart attack.
But I cannot overemphasize it enough: GO TO CARDIAC REHAB.
Cardiac rehabilitation programs are staffed by doctors, nurses, exercise physiologists, physical therapists, dietitians, psychologists, and social workers to help you find an appropriate exercise routine, the best way to improve your fitness levels, and get back to your usually daily activities.
Most programs will provide you with three key elements for long-term success:
- Detailed education about your heart condition, risk factors, and lifestyle changes for good cardiac health;
- Supervised exercise sessions and education about how to self-manage your frequency, intensity, duration, and types of exercise after a heart attack; and
- Recommendations for exercise after you complete cardiac rehab and suggestions for ongoing follow-up care (how to prevent another heart attack).
Home-based and hybrid cardiac rehab
Hospital-based cardiac rehab may not be feasible for everyone due to geographic limitations, so home- and hybrid home-hospital based programs have shown promise.
A recent systematic review and meta-analysis in the Journal of the American Heart Association found that home-based cardiac rehab and hybrid cardiac rehab improved functional capacity and are viable alternatives for those not suited to clinic-based cardiac rehabilitation.
Can I exercise after a heart attack?
The short answer, generally speaking, is yes, you can exercise after a heart attack.
A big YES.
You CAN and SHOULD exercise to improve both your heart function and general health.
But before you exercise either in cardiac rehabilitation or on your own, you must be certain you receive clearance from your cardiologist and/or surgeon (if you’ve had cardiac surgery).
Depending on the condition of your heart and your individual medical history, your doctor may want to perform a treadmill stress test on you just to be sure that your heart is stable enough to withstand regular exercise training (plus it gives you peace of mind too!).
When can I exercise after a heart attack?
The time it takes to get back to exercise after a heart attack will vary from person to person, but you can generally get moving within a day or two after surgery.
While you’re in the hospital, the nurses will probably want to get you up on your feet and have you doing laps around the nurse station at a very low intensity (i.e., snail pace, just one foot in front of the other).
You’ll likely do multiple bouts of, say, 5-10 minutes at a time.
Once you leave the hospital, you’ll probably be able to carry on with your low-intensity home exercise until your follow-up appointment with your cardiologist (or surgeon).
This will likely be around 3-4 weeks or so.
You MUST remember that even when you start to feel better, after any heart episode and surgery, there is still healing happening on the inside.
A heart attack inflicts trauma on the heart and, if you’ve had any damage to the heart muscle, then your ability to exercise may be compromised.
Only your doctor can tell you the extent of heart damage (if any).
As mentioned above, cardiac rehabilitation sessions are also advisable, as this allows you to “test drive” your ticker under the watchful eye of a trained cardiac nurse and exercise physiologist.
Provided you are asymptomatic (no shortness of breath, no chest pain etc) and have no heart rate or rhythm abnormalities on the electrocardiogram, then you will likely be fine to get back to (or start) your exercise regimen.
Benefits of exercise after a heart attack
The benefits of exercise after a heart attack are not too different from those in people who’ve not had a heart attack.
Though the main point of difference is a particular focus on improving the function of the heart, particularly if there was any damage to the heart muscle itself.
In other cases, some people experience what is known as “stunned myocardium” which is where the heart muscle is not dead, per se, but is injured and may regain some of its contractile properties after a few weeks.
Finally, it is possible to have a heart attack yet not have any damage to the heart muscle – often when treatment is administered soon after the onset of symptoms.
Reasons to exercise after a heart attack
Improved heart function
Regular exercise training helps improve the heart muscle’s ability to use oxygen, resulting in less demand on the heart and a reduced likelihood of future symptoms of angina
Improved body function
This is a simplified way of saying that your exercising body becomes more efficient at extracting oxygen from the blood and using it down at the cellular level (i.e., in your exercising leg muscles). The benefit of this is that your heart doesn’t have to work as hard
Reduced cardiac risk factors
Exercise can help reduce body fat, increase valuable muscle (increase your metabolic rate), reduce blood pressure, improve cholesterol and triglyceride levels, and reduce your risk of developing type 2 diabetes (or help improve your blood glucose control if you’ve already been diagnosed)
Reduced risk of a second heart attack
Following on from above, exercise can minimize your risk of having a second heart attack. Life can be unpredictable sometimes and you never know when you’re going to have to exert yourself, so being physically trained is a great way to minimize the possibility of another heart attack
Improved psychological well-being
Exercise has anti-depressant and anti-anxiety effects on the body. It helps you burn off the daily stresses of modern living, and this is even more valuable after having had a heart attack
What’s the best exercise after a heart attack?
The best answer is: it depends. On you.
There’s no set in stone rule for which exercise is best after a heart attack, but walking and cycling are quite commonly recommended because they’re practical and easily accessible to most people.
For people that have had a stroke and may not be able to take up walking, arm-based exercises such as an arm ergometer (arm crank) can be a great way to get the heart rate up and challenge the heart to get stronger.
If you have arthritis, the amount of activity you can do may be limited by pain, so water aerobics may provide the exercise benefits but without the stress on your joints.
Weight training (resistance training) is also a viable form of exercise after a heart attack, but it is advisable to build a good cardiovascular exercise base first and then add the resistance training when you’re feeling stronger and have received clearance from your cardiologist.
Inpatient exercise guidelines
The “by the book” exercise prescription for in-patient exercise (still in the hospital) as set forth by the American College of Sports Medicine is as follows, but I will also provide a bit of additional explanation.
Frequency
Early mobilisation
Two to four times per day for the first three days of the hospital stay. This may include a short walk for short distance. Depending on your energy level, you might even find 5 to 10 minutes of walking to be tiring.
Later mobilisation
Two times per day beginning on day four of the hospital stay with exercise bouts of increased duration.
While it’s true you need your rest, bed rest is also the single worst thing for your body.
Remaining flat on your back in bed can cause stiffness, constipation, and lost of strength.
The nurses will probably get you sitting up and walking around your hospital room just to place some gravitational load on your body.
Intensity
Suggested upper intensity limits:
Heart rate of 120 beats per minute or less; OR resting heart rate plus 20 beats per minute as the arbitrary upper limit.
Be aware that medications such as beta-blockers (i.e., metaprolol) will lower your heart rate so the numbers may not be an accurate indicator of how hard you’re working.
Even so, it’s still not a bad idea to keep tabs on your exercise heart rate so you know what your individual response is under the effects of your medication regime.
If you have a hard time finding your pulse, get yourself a heart rate monitor or a Fitbit (which also tracks your non-exercise movement habits).
Focus instead on a self-perceived intensity level of light to moderate exertion. If you find yourself short of breath, then cool your jets and ease up a bit!
Time (duration)
Perform short, intermittent exercise bouts of three to five minutes as tolerated. Incorporate a slower-level walk between bouts or rest if you feel this is necessary (go by how you’re feeling or your energy levels).
The general rule immediately after a heart attack is more exercise bouts per short duration, then ween yourself onto longer durations while reducing the number of exercise bouts until you’re doing at least 30 continuous minutes of exercise at a light to moderate intensity (see above comments on intensity).
It is important to understand that these are general guidelines and may not be appropriate for you depending on the extent of damage from your heart attack (if any), medications, and other medical considerations.
Discuss these recommendations with your nurse or cardiac rehabilitation team to find the right inpatient exercise prescription.
Outpatient exercise guidelines
The following post-heart attack exercise prescription is appropriate for when you’ve been re-evaluated by your cardiologist and/or surgeon and have been cleared for more vigorous exercise.
Frequency
Strive to perform at least four days per week and work up to daily (7 days per week).
Intensity
If you’ve had a follow-up treadmill stress test performed by your doctor then, depending on your level of conditioning, you might want to start off as low as 40% of your measured max heart rate up to as much as 80% of your heart rate.
This is casting a wide net, so it really will have to be tailored to your individual needs.
As mentioned above, if you’re on beta-blocker medications, then your heart rate may not be an accurate reflection of your intensity.
Instead, aim for a self-perceived exertion in the window of “light to moderate to somewhat hard.”
If you have the opportunity to exercise at a cardiac rehabilitation program, then you will likely receive specific guidance for monitoring your exercise intensity.
Bottom line: take it easy at first and then gradually progress yourself to higher intensities, paying particular attention to the onset of any signs or symptoms (shortness of breath, dizziness, etc).
Time (duration)
Give yourself a light 5 to 10 minute warm up consisting of light walking and stretching.
Depending on your level of conditioning (or deconditioning), aim for 20 to 60 minutes.
The obvious implication here is shoot for the lower end when you’re just starting out and progress to 60 minutes as tolerated.
Increase your duration by around 10 to 20 percent per week, though this will have to be tailored to you depending on how fit or unfit you are.
Remember that exercise isn’t all just about your heart and lungs.
Also pay attention to localized fatigue in your legs. If your lower extremities experience fatigue, then just slow it down a bit or take a break.
You’ll find with regular training that you can go longer and longer each week throughout your recovery.
Type of Exercise
As mentioned above, walking and cycling are probably the two most common types of exercise due to their easy access.
They engage the large muscles of the lower body which helps maximise the amount of energy (calories or kilojoules) you burn which in turn helps you lose weight and keep it off.
Other forms of aerobic exercise may include:
- Arm ergometer (arm crank)
- Combined walking/cycling with the arm ergometer (combined upper/lower body workout)
- Elliptical trainers
- Rowing machine (rowing ergometer)
- Stair climber machines
- Aerobics classes such as step class or newer crazes like Zumba
The bottom line is find a form of exercise that you enjoy and are more likely to stick with.
Find an exercise buddy and keep each other on the straight and narrow.
For more information, see my post on “yo-yo exercise” and how to stay on track with your exercise regimen.
Strength training (resistance training) after a heart attack
You can perform resistance exercise after a heart attack, though I strongly advise you to first build a solid aerobic exercise foundation and get clearance from your cardiologist (particularly if you have high blood pressure) before pushing any heavy weights.
Strength exercises may include free weights, machines, or rubber resistance bands. With regular training adaptations, strength conditioning can help you manage strenuous activities with reduced load on your heart.
Though not set in stone, our cardiac rehab team recommended approximately 6 to 8 weeks in cardiac rehab before we’d allow anyone to undertake any heavy lifting.
But for the most part, lighter weights may be a good idea just to help you learn the movement patterns and develop proper technique.
In the beginning, aim for at least two to three days per week lifting weights that permit around 12 to 15 repetitions, and performing 2-3 sets.
Be sure to EXHALE as you’re lifting the weight against gravity (remember: EXhale on the EXertion).
Or when in doubt, do NOT hold your breath, as this may increase your blood pressure.
If you carry a lot of fat around your belly, some exercises might need to be modified if your midsection impedes your range of motion.
I would suggest working with your cardiac rehab exercise physiologist for specific guidance on resistance training. While the benefits of weight training are clearly established, if not done properly it can lead to injury and possibly further cardiac complications.
Alternatively, send me an email and I’ll do my best to steer you in the right direction.
Yoga and Tai Chi
Yoga and Tai Chi can help you improve your activity level and resume your usual active life.
Yoga
Gentle yoga is unlikely to cause any problems, but if you had open heart surgery after your cardiac event, yoga could place stress on your sternal incision site.
Other types of yoga like hot yoga could potentially cause your blood pressure to drop. If you’re on blood pressure lowering medications, then the effect could be compounded and put you at higher risk of fainting. Speak to your doctor for clearance and make sure your yoga teacher knows about your medical history.
Check out this article by Johns Hopkins Medicine for more information on yoga for heart patients.
Tai Chi
New research has shown that for people with heart problems, Tai Chi can improve quality of life and lower stress, anxiety, and depression.
Tai Chi has been shown to lower blood pressure and lower cholesterol, body weight, and improve C-reactive protein (a marker of inflammation in the body).
For further reading, here is a link to the medical journal Medicine on Tai Chi and heart health.
Take home message
The bottom line is that exercise after a heart attack is safe, beneficial, and advisable in most cases. Provided you are medically stable and have received clearance from your doctor to return to exercise, you should be able to regain your fitness level.
Cardiac rehabilitation is an important intermediate step to returning to exercise as safely as possible.
The best advice is to work closely with your cardiologist and cardiac rehab team for guidance specific to your condition.

How much damage is done when exercise after a heart attack is delayed 4 months ?
Hi Pam, It is unlikely you’d do any more damage to the heart by delaying exercise for 4 months after a heart attack. Though it’s fair to say doing nothing isn’t going to do the heart any favors either. Heart attacks and subsequent damage to the heart muscle can vary from person to person depending on how large and deep the infarct was. Naturally recovery times will vary too and the time it takes to get clearance for exercise will depend on the cardiologist. Was a surgical procedure done after the heart attack? Bottom line: a lot of factors to consider in determining how long one should wait before getting into exercise. I would suggest getting in touch with your doctor to see about getting a referral into cardiac rehab. This way they can hook you up to an ECG while you’re exercising to ensure you’re ticker is responding normally under exercise stress. Hope this helps. Best wishes.
Can I cause heart damage by one day straining with heavy physical exertion at work approximately 3 weeks into my cardiac rehab? This was after an episode with tokotsuba syndrome. I was doing very well as I am 60 and in pretty good shape but then my BP really spiked on that day and had a hard time bringing it down again. Working with my Dr and resting more now and understanding my limits. Thanks!
Hi James,
In general, if you’re recovering from any cardiac event, it’s best to heed the specific instructions from your doc regarding your recovery. It’s theoretically possible to cause damage from heavy physical exertion (as can happen to people who are, for example, shovelling heavy snow and then have a heart attack). Once your heart rate and blood pressure are well-controlled and under your doc’s supervision, then you’ll probably be able to get back to exerting yourself again without any worries. Bottom line: work closely with your doc and let him/her know all of your concerns. Kind regards, Bill
Hi,
What core exercises are safe to perform after 2 heart attacks. Cardio has been the main focus but not done any work on the core and upper body.
Thanks
Hi Victoria,
Thank you for your comment. If you’ve had two heart attacks, my main concern as an exercise physiologist is that you are deemed by your cardiologist to be medically stable and well-managed (healthy lifestyle, taking meds as indicated). Did you have an angioplasty/stent or open heart bypass surgery? I would discuss this with your cardiologist and perhaps ask for a treadmill stress test to determine your exercise capacity. If you can tolerate relatively high workloads then you would likely be stable to perform weight training exercises at a low level and gradually progress to higher training volumes.
Most exercises are fair game provided you do not have any unstable aspects to your condition. For example, if you told me you had two previous heart attacks and were experiencing chest pain at rest (unstable angina), then obviously this is cause for concern and exercise could clearly worsen the situation. My advice would be to hire either an exercise physiologist or a personal trainer in your area to go over some core and upper body exercises with you. If you have underlying high blood pressure then you need to be aware of your breathing upon exertion (exhaling on the exertion). IF you’re holding your breath when lifting weights, this can increase your internal pressures which may cause a further rise in blood pressure and possibly predispose you to having another heart attack. Be sure your EP or trainer diligently monitors your heart rate and blood pressure response.
Again, going back to my comments above, provided you are medically stable and reasonably low risk, you should be able to tolerate most exercises reasonably well. Be aware that it would be inappropriate for me to provide specific advice given that I am not familiar with the intricacies of your medical history and situation. I hope this helps move you in a positive direction.
Cheers
Bill
I had an MI 8 months ago,and was very active before and the day of the MI but could not beat DNA (Father died @ 48 sister @ 60)I’m 55 without any additional morbidity factors. I am now riding a mountain bike 12 to 20 miles 6 days a week.I went through cardiac rehab successfully (I recommend it to everyone)My max Heart Rate has been 153 so far. Can I go safely up to 170? After my stress test the Cardiologist told me that I should be able to do that in bursts. Just curious as t your thoughts.
I had a heart attack 2 months ago. The surgeon put 2 stents in the left artery. I’m 52 but I’m in good health. Normally I have sex 2 times a day. Is it ok for my health? Please tell me.
Hi Guna, You’ll need to discuss this with your doctor, but provided you’ve had a stress test and was able to tolerate a reasonably high intensity, this should be a fairly good indicator that you can return to sex. If you had damage to your heart muscle then this could potentially complicate things, but again, bottom line: speak with your doctor to get clearance.
Dear Doctor Bill,
I just had open heart surgery December 7th, 2012 to replace a bicuspid valve. At 54, 150 pounds I am in pretty good health except for needing that done. I was up walking around the hospital the next morning and continued that three (2) times a day until my release after only four (4) days. Trying to walk now around our cond’s three (2) times aday as I begin to heal. How soon will I be able to start some other kind of physical therapy and where can I find what type of things I can do?? PLEASE need to know, since I wont be able to afford physical therapy with my insurance starting over again in a few days. I have to get back to work soon and have to do the best I can, as soon as I can.
Sicnerely,
Terry Dean Hallgath-Boyd, Nashville, TN
Dear Terry,
Thank you for your message. Sounds like a quick hospital course for you. Most open heart procedures will keep you in the hospital for at least 5 days, sometimes up to 7 days. The fact that your reasonably young and are clearly not overweight is only to your advantage. Also remember that valve disease is generally a separate entity unrelated to arterial disease (plaque in the arteries). Perhaps you had rheumatic fever as a child which can sometimes translate to valve problems later on. In any event, it’s still a concern, but less likely to kill you than coronary artery disease.
As for when you can start an “alternative” physical therapy, this will depend on your individual situation. Because this is just a website and I’m not familiar with your detailed medical history, I cannot legally give you specific advice. I can certainly appreciate your situation being a victim of the US health insurance cartels. I cannot tell you how many times I wrestled with them to get coverage for my patients. It is criminal.
Anyway, as for your situation, consider the following:
1) you are still pretty well fresh out from under the knife. You need some recovery time. In my experience, most uncomplicated surgeries will require about a month or so until you’re reasonably healed up to start doing more strenuous activity. You have to consider your sternal incision and that your breast bone needs to heal, so no pressure on this.
2) You will likely have a follow up appointment with your surgeon (who wants to see his handy work is healing well) and your cardiologist who is likely going to want to run some tests on you to make sure your heart is working properly. I suggest speaking to them about getting a referral into a cardiac rehabilitation program. This is not physical therapy and may possibly be covered by your insurance company. No promises but worth a try.
3) During your first month of recovery, refer to the general guidelines in my exercise after coronary artery bypass surgery. They’re generally the same for any open heart procedure: Coronary Artery Bypass Surgery Exercise Guidelines . You need to at least be up on your feet and doing what we call “activities of daily living.” It may not seem like exercise, and it’s not, but it is indeed physical activity that counts. You need your bed rest but you also need to be upright and gravity bearing too.
4) Once you get clearance from your cardiologist that everything is healing well, then I’d suggest perhaps finding a clinical exercise physiologist in your area, ideally one with EXPERIENCE with cardiac clients, and get some general guidelines for exercise. It might even be worth a few sessions. Even if it costs a few hundred bucks, you’ll at least have some good quality recommendations to go on.
Bottom line:
Once you’re cleared after a month or so, and provided you’ve been doing your light exercise plus activities of daily living, then you should be ok to start engaging in proper structured exercise. Get guidance from a qualified (masters degree level) exercise physiologist. If no signs or symptoms, then you can start increasing your intensities. Again, apologies for not being able to answer a lot of specific questions, but I cannot legally do so unless you’re under my care and I am familiar with your entire medical history. Hope this helps.
Best wishes,
Bill
Hi Bill, I just had a serious heart attack with 4 stents put in. I was told I only had an ejection fraction of 24 percent where a normal person has 60 percent. Will this number increase in time had surgery Feb 14 2019. I still can’t get my energy back thanks
Hi Bobby,
I can’t really give any specific medical advice over the internet, but I can give you some information that you might like to discuss with your doctor.
It sounds like it was a big heart attack if your ejection fraction is down to 24%. Since your surgery was only on 14 February, it is still early days in the recovery period. You might want to ask your doctor about your troponin levels, which give an indicator of damage to the heart muscle. Find out how high your troponin levels were and ask how much damage was done. Also ask if this damage was something permanent or if your heart muscle will recover and regain a bit of that lost ejection fraction.
Also remember that your body works together as a system. Even if you have some permanent damage to your heart, over time, as you do regular exercise, you can improve the efficiency of the rest of your body. For example, your muscles become more fit and efficient at extracting and using oxygen and nutrients from the blood which means that whatever blood is being pumped from your heart, your body will be more efficient. This can help you feel a bit more normal and not so tired all the time.
As for being tired right now, this is quite common after such a major cardiac event. If you told me you felt great, then I would think something was terribly wrong. Not many people feel great after a big heart attack and four stents. Try to be patient and give yourself permission to be human and recover.
If you are feeling anxious and stressed, I would recommend getting a referral to a social worker or psychologist with experience working with people with medical issues. It’s some real scary sh*t and if you feel worried, then that’s pretty normal. But there are trained professionals available to help you through this. I would strongly encourage you to seek out help if it’s impairing your ability to live your life.
Hope this helps.
Kind regards,
Bill
Thank you really appreciate it love your site very helpful.
Hi,
Is it possible to have had a heart attack and have no permanent damage. I had a MI nearly two years ago now and was convinced it was mild indigestion. I started to feel nausea with it and that is what made me drive myself to hospital. I had no pains or anything “Hollywood” about my heart attack. Quick two days in hospital with an angiogram and told to give up smoking (which I did instantly) I am on the standard medication and have no angina or anything else that would be common. I exercise hard and eat well staying away from high sat fat food as best as possible. I feel better than I did before my heart attack and consider it in a perverse way a blessing in disguise.
Hi Dr
I had a heart attack in October and had a stent put in , I used to exercise 6 days a week ( 3 days of at least 5km road runs and 3 days of 30 – 40 minute intense bodyweight training sometimes with light dumbbells ) , when should it be okay to get back to my exercise regime ? Should I ask my cardiologist for a exercise stress before I start ? I currently only walk .. And even though I have adjusted my diet which was good to begin with I have gained 3 KG since the event.. When I asked this questions from my cardiac rehab they didn’t give a clear answer
Hi Manisha,
Thank you for your message. I know it can be frustrating wanting to get back to your old level of exercise after a heart attack. In answer to your question, I think it’s a good idea to discuss an exercise stress test with your cardiologist before you resume heavy exercise. Depending on the level of damage to your heart muscle (if any), you must be aware there is still healing taking place on the inside. I would imagine by now that since you are a few months post-op, your doctor might be amenable to giving you a stress test. You will want the piece of mind in knowing that your heart is strong enough to withstand the higher intensity exercises without any limitations in oxygen flow to your heart muscle. Provided your cardiologist is satisfied with your performance, then you should be able to cautiously return to your higher intensity workouts. Best wishes in your exercise pursuits!
Hi Dr Bill
Thank you for replying toy previous query , it’s been 5 months since my angioplasty , and I have started exercise also done a stress test as advices by you. It was done for 15 minutes and my cardiologist mentioned that there was no visible damage to heart after test. I am still a bit reluctent to start strenth training ( body weight ). Is it okay to do pushup variations, burpees ect. I still have occational heart burn. Although my cardiologist says it has nothing to do with the heart.
Hi Manisha,
Thank you for visiting my site and leaving another comment. If you were able to tolerate a solid 15 minutes of a stress test and your cardiologist told you the heart was looking strong, then that is a very good sign. If you did not have any damage to your heart muscle, then it’s fair to say you had more of a plumbing problem (blocked arteries) than a heart problem (heart muscle damage).
It is completely normal to be a bit hesitant to get back into strength training after a heart attack. Provided your cardiologist has given you the all clear, then I cannot see any compelling reason for you to not ease back into a weight routine. If you’re using your body weight as resistance, then I can’t see that pushups and burpees will give you too much of a problem. You must just be sure to pay attention to your signs and symptoms along the way. If you are feeling any sort of pain that is out of the ordinary and not what you’d expect to feel from weight training, then you should heed these symptoms. For example, it’s normal for your muscles to feel fatigued and maybe a little sore in the day following exercise, but if during exercise you are exerting yourself and feel the standard angina symptoms like squeezing in your chest, pain down the left arm, profuse sweating beyond what you’d expect with exercise, etc, then those are the kinds of symptoms you should report to your doctor. If they don’t go away on their own with rest, then you should get yourself to the hospital.
In closing, again, make sure you discuss this with your cardiologist and get his/her approval to do resistance exercise. When you do, just be sure to ease into it and gradually progress to higher intensities over time. Watch for signs and symptoms that do not appear to be exercise related and you should be fine. Bottom line: be cautious and aware! Best of luck.
Hi Manisha
Here’s a quick link to an article I just wrote on exercise after angioplasty and stent. I hope you find it helpful: https://drbillsukala.com/exercise-after-angioplasty-stent/
Thank you once again.i must say i have been a regular visitor to you site and find the content very informative .
Thanks for the kind words Manisha. Most appreciated!
Hi Dr Bill.
Just a quick query from a UK user of your great site;
On March 19th I had an M.I. and then 2 cardiac arrests in the ambulance, then a stent fitted and balloon pump running for two days, was released after 4 days. Now on Asprin, Clotbusters, Beta Blockers, ACE inhibitor and a Statin. Am 41 and 97kg was healthy and semi fit before and MI happened when MTB’ing.
Have been resting, exercising lightly, (walking and cycling) and doing a basic, (older person centric) group rehab. Have now been prescribed a Gym based training scheme.
Looking to get very fit and have a target 100Mile offroad MTB ride July 2016 for Heart Charity
Just nervous ahead of stepping up to proper, modern fitness training and diet plan, am unsure of what best approach to the problem of caution vs actually working hard enough to do any good.
Any advice for shaping my program/plan? Also building confidence in Heart again?
Many thanks
Dave F
Hi Dave,
Thanks for leaving a comment. I think the first order of business is to make sure that your heart is fully healed after the heart attack. Did the docs tell you if you had any damage to the heart muscle? If you’ve had damage to the muscle or what is known as “stunned myocardium” then it may take a bit for your body to readjust. It looks like you’re about two months post event now and that, in my experience, generally tends to be a good time to start moving back into an exercise regimen.
When you did the cardiac rehab, did they hook you up to an ECG while you were exercising? If so, were there any arrhythmias? If so, what types of arrhythmias were they? The occasional premature ventricular contraction is not generally considered a big deal, but if you get a lot of them and of different shapes, then it might be something for the doc to investigate further.
Once you’ve been fully cleared for exercise, then you’ll need to follow good prudent exercise guidelines such as making exercise predictable (initially) and then working up to higher intensities. This way you can define what intensities elicit symptoms (if any). You are still pretty young in the grand scheme of things, so remember that your peripheral improvements (i.e., your exercising muscles) can help compensate for the heart. In other words, the more fit your body is, the easier the workload on the heart. Plus you will improve the strength of your heart muscle with regular activity.
I would suggest finding a qualified exercise physiologist in your area with experience working with cardiac clients and then have him/her help guide you along. Obviously I’m on the other side of the world, so without knowing the full details of your medical history and the heart attack, I could not give specific advice. But as a general rule, I would suggest easing into it and being vigilant about any signs or symptoms. You might also benefit from having a treadmill test done by your cardiologist to make sure you’re able to do the high intensities without any abnormalities on the ECG which may or may not be accompanied by symptoms.
Feel free to write again and let me know how you’re going.
Kind regards
Bill
Hi Dave,
Here’s a quick link to an article I just wrote on exercise after angioplasty and stent. I hope you find it helpful: https://drbillsukala.com/exercise-after-angioplasty-stent/
Hi Dr Bill
I am a post graduate student doing research on stents and the effects of exercise on clients with stent.
The aim point of this study is to show that although these cardiac have stents that its important to engage in a 12 week exercise intervention in order to further unblock arteries.
Hi Dr Sukala,
i am 54, i visited the hospital with chest pain and the doctors said that it was angina. I had an angiography and had double stenosis on LAD artery, so i had angioplasty and two DES stents were put in my artery, with “excellent final result”, according to the doctor’s report. This was about a month ago.
As i did not suffer a heart attack, can you please tell me how i should consider my condition?
I do have a few extra kilos, which i already work to get rid of, i continue to walk about forty minutes every morning as i used to do (from week 2 after the angioplasty), and now i would like to start lifting weights, is this ok?
The fact that i did not suffer a heart attack and accorging to the doctor i do not have any damage on the myocardium, how does this affect my current condition.
Finally, please accept my congratulations for your very informative website, but mainly for the fact that you spend form your (precious, i am sure) time to answer our questions.
With my best regards from Cyprus.
Hi Charis,
First off, congratulations on taking the correct steps in getting to the hospital as soon as you had chest pain. Time is heart muscle so had you not gone to the hospital when you did, it could have progressed to a heart attack.
As for your condition, because you did not have a heart attack, you essentially had a “plumbing problem” and not a “heart problem.” However, this is an excellent opportunity to work on risk factor management.
If your hospital has a cardiac rehabilitation department, then you might consider enrolling in the program for them to help guide you with your exercise. Since you are a month post-stent, this might be a good time to speak with your cardiologist to see about getting approval to start lifting weights. As you can appreciate, I am unable to give anyone specific advice because there is no way I can fully know/understand each and every person’s condition. Each situation is unique despite the similarities. Bottom line: get approval from your doc before you start pushing yourself.
I would also suggest speaking to your cardiologist about giving you a treadmill stress test to examine your heart function under high intensity exercise. If you can tolerate several stages of the stress test and there are no abnormal changes on the electrocardiogram, then they might be more likely to give you the green light to start lifting weights.
I would caution you that if you’ve had blockages in the LAD then there is always a “possibility” that there could be blockages in other arteries that are not yet giving you symptoms. Pay attention for any signs or symptoms similar to the angina you previously had. Again, I would suggest working on risk factor management through your hospital cardiac rehab (if available).
Also keep an eye on my blog because I’m about to publish a new article specifically focused on stents and exercise.
Thanks for visiting all the way from Cyprus!
Kind regards
Bill
Dear Bill,
thank you very much for your answer. I understand that you cannot give specific advice, and i keep what i believe is the bottom line from what you are writing me: as i avoided the heart attack, now is the time to minimise the risk for a new artery blockage, so reduce my weight, give up smoking and live a healthier life.
Regarding your new article, it will be very interesting indeed, so i look forward.
Last but not least, yes, Australia is so far away from Cyprus, but with half my family living there, is a place i always have in my heart 🙂
Once again thank you so much and wish you all the best.
Dear Charis, thank you for taking the time to write back. I think you’re on the right track. It’s just a case of making those lifestyle changes and sticking with them for the long term. Sending you lots of positive vibes from Australia. Maybe we’ll see you down at Bondi Beach on your next visit! Cheers mate!
Hi Charis,
Here’s a quick link to an article I just wrote on exercise after angioplasty and stent. I hope you find it helpful: https://drbillsukala.com/exercise-after-angioplasty-stent/
Dr Bill,
I’m a 51 year old male who had a heart attack while I was bench pressing in the gym. Fortunately, I called 911 and was taken immediately to the ER where they inserted 3 stents (two for the LAD). It’s been 3 months since the procedure, and I’ve been to cardiac rehab and cleared by my doctor to go back to the gym. I’ve switched to a low-sodium/cholesterol/fat vegan diet and now walk 3 miles a day. Mr doctor believes I had a plaque rupture while I was bench pressing a very heavy weight, and that formed the blood clot in my LAD. So my question is, will I ever be able to go back to lifting heavy weights again? Or, should I stay with lighter weights and higher reps for the all future workouts? Thanks.
Hi Dave,
Thanks for sharing your experience. Looking at all the info you’ve provided, you’re clearly on the right track. My view is that people who are active that have heart attacks SHOULD do cardiac rehab to make sure ticker is ok to get back into exercise again. So you’re ahead of the game there. I think when it comes to situations like yours, it’s a case of sometimes bad things happen to good people. You do everything right, you go to the gym, try to stay healthy, and then these things pop up and alter your life. From my work in cardiac rehab, it’s not as uncommon as you might think.
In answer to your question of whether or not you’ll be able to lift heavy weights again, this is something you’ll really need to discuss in detail with your cardiologist. When it comes to coronary artery disease and heart attacks, sometimes it’s better the devil you know than the one you don’t know. Your proverbial volcano has already erupted, so at least now you should have a bit more information from the cardiac catheterisation about where your blockages are. You’re probably on meds that will help reduce your blood pressure and overall cardiac workload. This could help minimise your chances of another event.
I would suggest talking to your cardiologist and asking him/her if there are other plaques in any other arteries (i.e., RCA, left main, circumflex etc) which might be susceptible to rupture if you go back to lifting. Speaking of lifting, as you are now probably acutely aware, weight lifting can cause massive spikes in blood pressure, particularly during valsalva (breath holding). I would venture to say you had an unstable plaque that just couldn’t handle the pressure which is, obviously, what resulted in an acute MI. The good news is that now that you’ve been treated and it’s been three months, it’s probably unlikely the same arteries would occlude again. It’s possible they could plug up again (theoretically) but provided you have angiographic evidence that the angioplasty/stents worked, then the probability of another MI is low(er).
If you want to err on the side of caution, you might stick with lower weights that won’t cause such a spike in blood pressure. Legally I cannot give you any resolute yes/no, do this/don’t do that type of response. I’m hopeful that this information gives you something to go with to your cardiologist to have a discussion about future directions with your exercise. Kind regards.
Thanks for your comments and feedback, Bill. I do appreciate you taking the time to respond to my questions. Sometimes I do feel my heart is a “ticking timebomb” ready to go off anytime, but my cardiologist has assured me that I shouldn’t worry about it. I am going in for a stress echocardiogram next month, so hopefully that will reveal the current level of healing of my heart. I will take your advice and speak with my doctor about lifting heavy weights, and will see what he says. Thanks again.
Hi Dave,
Here’s a quick link to an article I just wrote on exercise after angioplasty and stent. I hope you find it helpful: https://drbillsukala.com/exercise-after-angioplasty-stent/
I used to have my partner crack my back by standing on it to relive discomfort,but i had a heart attack and 4 stents put in 2 months ago,im at home now and i have the need to crack my back as its starting to annoy me,but is it ok to do it.
Hi Rick. That is one of the more unique questions I’ve received on my blog. It would probably be best to run it by your doc, but unless your partner is absolutely crushing you, I can’t imagine it should impact your stents. Best wishes
Hi Dr Bill, my brother, almost 65, had a heart attack and four stents, with the possibility of needing another. He was in good condition before this happened. He ran five miles and did weight training all his life. He is a former miltary man and a police officer for 33 years. He is a bit OCD and has already started running and is only beginning his third week of recovery. He has not seen his cardiologist yet. Is it safe for him to be running this early? He is on Plavix and I believe he takes a beta blocker and baby aspirin. I wonder is he might be doing damage to the stents by running so soon. Any information you can give me would be greatly appreciated. Thank you, Donna
Hi Donna, thanks for your comment. I can’t say for sure if he’s doing any damage, but I do generally recommend that after a heart attack and intervention that people get clearance by their cardiologist before doing any high intensity exercise. In cardiac rehab we encourage patients to do light walking during their recovery UNTIL getting final clearance by the cardiologist to step it up to running. We used to say denial is not a river in Africa, and it was usually the men who were the biggest offenders with not listening 👂. He is on meds, so that should help keep his blood pressure down during exercise and minimise his risk of a stent failing. It sounds like he needs a baseball bat of reality across the back of his head, but you know how some people are. They’ll do what they want no matter what. Bottom line: he is increasing his risk by pushing it too soon. If he can do a cardiac rehab program with telemetry monitoring, they’ll be able to let him know how his ticker is looking in terms of heart rate, blood pressure, and arrhythmias at the intensities he is currently doing. Hope this helps. Kind regards, Bill
Hi Dr Bill,
Finally my search for do’s and don’ts after Angioplasty ends here. Really very helpful.
Thanks for the Valuable information and services.
No worries Bhanu. Glad you found this helpful.
Hi I’m 41 years old had an heart attack 2 weeks ago they put one stint to open my 97% blocked altary. I always lifted weights since I was I kid. My question is that I can still lift weight? One of my friend said I can’t because when we lift weight stint can move to heart. Please advise my doctor told me I can have normal activities after two weeks
Hi Sahil, thank you for your comment. If you’re only 2 weeks after your stent, this is quite early for lifting weights. You still have healing happening on the inside both from the heart attack and stent. I would advise speaking to your cardiologist and perhaps ask him to do a treadmill stress test on you at the 4 week point of recovery to ensure your heart is stable with no rhythm disturbances (arrhythmias). Assuming all is normal, then you should be ok to ease into weight lifting again.
Can we play football after a cardiac arrest? Plz tell.. ?? 🙁
Hi Vishnu, you’d have to speak to your cardiologist to be sure your heart is stable enough to play football. Ask your doctor for a stress test and if you can tolerate high workloads then this may be a good indicator you can return to football. But you will ultimately need your doctors approval. Hope this helps. Kind regards
Hello and thanks for all the valuable honest information about the heart problems and sports!
I have some questions, for which I didn’t really receive an answer from my cardiologist. Here’s my background: I am 39yo male and had ST elevation infarction + stroke last December almost a year ago. They put a stent into LAD-B artery and I lived to see the next day. According to my papers, they found my other arteries ok. I had no cholesterol problems, no family history, no significant overweight, no smoking etc. Finally the reason was found: I have essential thrombocytemia – my platelets are always high. They were ~690 at the time of the MI. Now I am getting treatment, thrombocytes are down to 490 and hopefully getting lower etc. The stroke was discovered later, small scarring in cerebellum, makes my balance bit off occasionally but otherwise very mild stroke. Stroke was decided to come off from the clogs during the infarction. But this is not the issue here.
I have done power lifting for a long time. Not very good at it but a hobby of mine anyway. No drugs or any other hormones, ever. My cardiologist told me to stop doing “heavy weight training” and said he does not recommend it to anyone – even healhty. But he did not tell me WHY. What could possibly happen? My blood pressures are at most 130/70 and at home they drop to 100/55 with pulse of 50-60. I do also running and I did test my heart rates all by myself – and was able to get it as high as 160-170bpm. Did not feel ill, bad and no pain. I also started ignoring my doc and tried some medium heavy lifts. But the problem is now that right after a heavier single lift, my blood pressures drop and I feel very dizzy. I am eating ACE inhibitors, beta blockers + ASA and Plavix and I suspect that all the pressure problems come from the medication. Is this dizzines by any means dangerous (ignoring the possibility to fall)? Blood pressure of course goes up and down, but since the cholesterole is ok, heart seems to be able to pump and I did not have excess build up of plaque – what could go wrong?
I am planning in future to talk to another cardiologist about the meds too. If I don’t and did not have high blood pressure…then why am I taking the medication which makes me dizzy.
I asked the neurologist who checked me after the stroke, and he said there’s no limits in anyway for any sports. Still I always get a bit anxious when I get dizzy in the gym. Some of the dizziness comes from the anxiety itself!
Thank you again for the good forum!
G’Day Jarno,
Thank you for taking the time to leave such a long and thought out comment. Regarding your blood pressure changes, you should remember that even with no underlying medical condition or medications, a common and normal (expected) response after exercise is a drop in blood pressure, sometimes to a level lower than what it was at the start of exercise. This is due to your blood vessels dilating to accommodate more blood flow to the working muscles. When you stop exercise, your blood vessels remain dilated but there is no longer any demand on the muscles. So you get a bit of an enhanced drop. In my work in cardiac rehab, I commonly worked with patients who were (like you) on a cocktail of medications that affected blood pressure (including ACE inhibitors and beta blockers). So you can sometimes get a double whammy effect where your blood pressure drops down a bit lower from the combined normal response and the effects of the medication. This would explain your dizziness.
Have you tried drinking more water? This might help to increase your blood volume a bit and minimise the extent to which your BP drops out.
I agree with your decision to speak to another cardiologist. I’d suggest trying to find one who is an athlete him/herself and understands your situation. I’ve worked with many cardiologists over the years, some more understanding than others regarding exercise, and you do need to find one that is right for you. No foul there.
I apologise I cannot give a comprehensive exercise physiology consult here without your entire medical history.
Keep in touch and let me know how you go with your second cardiologist! Kind regards, Bill
Hello. I am 55 year old male i have been a runner for 7 years. On Oct 1st i had a heart attack while running on a treadmill at the gym. 95% blockage in the main artery “widow maker” they called it, don’t like that term. Two days in the hospital, 3 weeks cardiac rehab they released me from rehab 7 weeks early no heart damage. I am back to the gym running at 85% of max heart rate with wrist monitor. My question is i am doing a 5k i one more month that will be 10 weeks, should i pace based on 85% of max or can push beyond that?
Hi David,
Thanks for your comment. Sorry for the delay but I’m overseas on business at the moment so have not been able to sit down and respond properly. Before I begin, please know I cannot legally provide any specific advice for your situation, but I am happy to address some points that may be worth discussing with your cardiologist.
First, from one athlete to another, I can appreciate your eagerness to get back to exercise. I’m not a very good patient either, so I can empathise. But you do need to be cognisant that there is healing going on inside you (even if you feel great).
You state your heart attack was on 1 October. I generally don’t recommend too much strenuous exercise until at least 2 months or until cleared by the cardiologist. I’m guessing if you had a 95% blockage in your left main artery (the widow maker), then they probably did an angioplasty/stent procedure on you (is this correct?). If it was open heart surgery, you’d likely not be back at the gym yet.
Remember that 85% of your max heart rate is actually (more correctly) 85% of your theoretical max heart rate. Unless you know your MEASURED max heart rate then you’re just relying on the bog standard 220 minus age and then your percentages from that. So the actual heart rate could be higher or lower than your ACTUAL max heart rate.
Talk to your doctor and ask if it’s appropriate for them to run you through a max stress test. If you can push to max under the watchful eye of your cardiologist whilst on an ECG and there are no abnormalities in your rhythm or ST segment (ask the doc), then they might deem you stable for the higher intensities.
I’d say with reasonable confidence they would have done an angiogram on you. Ask your doctor the status of your other arteries. Were there any identified blockages in the left anterior descending (LAD), circumflex (CFX), right coronary artery (RCA) or other offshoots like the obtuse marginal (OM) or other smaller branches? Point is, you might be thinking your left main artery is your only concern but it’s possible they could have spotted other arteries that were blocked but comparatively quite low grade blockage (lower percent) and decided it wasn’t medically prudent at this time to touch those arteries.
If you’re on medications such as beta blockers, then they will reduce your heart rate to the point that you will unlikely reach your 85% max heart rate. In this case, you’d need to be looking at using the rating of perceived exertion scale (RPE). Ask the staff over at the cardiac rehab department and they can give you more of a run down on that (if necessary).
Hopefully this information helps give you some ideas of what to address with your cardiologist. Again, I never give specific advice over the internet since I don’t have access to your medical history, records, op reports, etc. Bottom line: talk to your doc, see about getting a stress test done, find out the status of your other arteries, and if possible, try and work closely with your local cardiac rehab department (particularly if they have an exercise physiologist there with extensive cardiac rehab experience).
Cheers
Bill
Had heart attack during sleep lost 45 per cent I walk 18 holes of golf no breathing problems I do elliptical 30 min have light sugar problem high blood preasure under control really can’t tell I had a heart aatack
Hi Ron,
Everyone has a different experience when it comes to a heart attack. Some people have small heart attacks and are debilitated. Others have comparatively larger heart attacks and still manage to get through life quite well. Glad to hear you’re doing well and not having too much down time as a result. Keep on moving! Cheers, Bill
I am 4 months post-MI and have completed a conservative 3-month cardiac rehab program. I now plan to run on my own but am uncertain of how intensely I can safely go (I like higher intensity exercise). Is the absence of arrhythmias during a graded maximal exercise test the gold standard for determining whether a post-MI patient patient can perform high intensity running? If so, how long are those treadmill test results valid for and when should I get re-tested? Also, what about very short duration (30 sec) high intensity sprints that are unlike a continuous treadmill test? Regarding high intensity weight lifting should I request physician supervised EKG monitoring during a graded resistance exercise bout to learn if that appears to be safe for me? Thanks in advance for your opinion.
G’Day Pat,
Thank you very much for taking the time to leave a comment. As I emphasise in most of my replies to comments, each and every person’s situation is a little bit different. In your case, you’ve highlighted that you did have an MI and also completed three months worth of cardiac rehab. When it comes to an MI, I often have a look at the extent to which there was damage to the myocardium (if any). I would look at the blood enzymes such as troponin I and T (see: https://patient.info/doctor/cardiac-enzymes-and-markers-for-myocardial-infarction) as well as an echo report which provided an ejection fraction. Provided you had a “small” MI and do not present with any significant wall motion abnormalities, then this puts you in a much better situation than someone who had half to 3/4 of their heart muscle blown out. Ultimately, I recognise that I am an exercise physiologist and always work in partnership with the cardiologist regarding specific recommendations for an individual that might not fall into neat and clean ACSM cookbook guidelines/recommendations.
Regarding arrhythmias during a GXT, first I think it’s a good sign if someone is able to achieve maximal effort without much more than “boring” old normal sinus tachycardia. Most people, even Olympic athletes, get the occasional PVC from time to time (no big deal). Unifocal PVCs are usually no concern but some cardiologists might pay more attention to multifocal PVCs (being propagated from various loci around the heart). If you’re getting short runs of PVCs and they’re asymptomatic, your doc might not be too fussed. However, if you’re getting long runs of them as VTach AND you’re symptomatic, then that would obviously require further evaluation. We used to catch people in VTach during cardiac rehab who were initially asymptomatic but after 3 minutes of sustained VTach became symptomatic.
If you’re an experienced runner and are still in reasonably good shape and your ticker is looking good after your MI (and angioplasty/stent if applicable), then your doc might green light you to go back to business as usual but might warn you to be hypervigilant in looking for signs or symptoms (shortness of breath, chest tightness, etc). If you’ve had a blockage in one artery, then there is a possibility there could be blockages in other arteries that have not yet been treated or are not yet on the radar. Most of the cardiologists I’ve worked with used the 70% blockage as a general guideline where they wouldn’t take action if it was low grade and asymptomatic. 70% blockage or higher and WITH symptoms during exercise would get some VIP attention in the cath lab!
I think with regards to all your questions (as a whole), I can’t give any specific guidelines since I’m not privy to your entire medical history, but I would strongly suggest discussing these questions with your doc (who is hopefully an exerciser him/herself). If they have you on meds like beta-blockers, ACE inhibitors, etc (all the usual suspects), then these may afford you some protection against very high HR and BP which might place particularly high stress on your ticker.
Bottom line: If you’re in reasonably good health, had no myocardial damage, could tolerate very high workloads on a GXT, had no malignant arrhythmias, were asymptomatic from start to finish, are on meds (as appropriate), then you could probably plead a good case to your cardiologist to get the final green light to go back to the high intensity exercise. Hope this helps.
Warm regards,
Bill
Bill,
Thanks for the thoughtful reply. Just to give you a bit more info, I did have a stent put in the LAD, the other arteries were relatively clean (< 20% blockage). I have had little in the way of arrhythmias during cardiac rehab, only an occasional PVC. One year before my MI, I happened to have a resting echo that showed left ventricular ejection fraction of 65%. The day after the MI the ejection fraction was 35%. I am taking a beta blocker (carvidlol) and ACE inhibitor (lisinopril), a blood thinner (Effient), aspirin and a statin. I am otherwise healthy. And I understand that your not a cardiologist and you don't have all my records. Nonetheless, an opinion from an individual such as yourself is helpful for me to better understand my situation. I will appreciate any further comments you may have. Cheers.
My name is Faizal, 49 yr old, had an angioplasty on December 26th 2014. I was a regular soccer player and had chest pain during a game. I was hospitalised and had 2 stents placed. After 5 months, I’ve started playing football again and am playing regularly without any problems for past 6 months. Can i continue my game? What precautions should i take?
Hi Faizal,
Thanks for your comment. First, it is a good thing that you were a regular exerciser going into your angioplasty procedure. This gives you a fitness base which is easier to maintain than build up after having had a heart procedure. It is also good that you respected your symptoms and took action. There are many people who have symptoms but ignore them or think they are related to heartburn or indigestion.
The big questions to consider here are:
1) Did you have a heart attack? and
2) Was there any heart damage?
If you had a heart attack, then you should speak to your doctor to see what, if any, damage occurred.
Based on the information you’ve provided, you seem to have had a solid amount of recovery time (5 months) so this is a good thing. If you’ve been cleared by your cardiologist for exercise and you’ve been playing football regularly for the past 6 months with no ill effects, then this is a good sign.
Regarding precautions, I would suggest that you be aware of any classic signs and symptoms like the ones you’d have experienced during your game. If you’ve had a blockage in an artery, it is still possible for the artery to reocclude (block up again) or you might have a blockage in another artery that was not treated.
Have regular check ups with your doctor and perhaps even ask if you can have a stress test to makes sure that your heart is looking normal on the ECG. This is not necessarily diagnostic, but the doc might pick up some early warning signs that could be used to warrant other more specific tests.
The bottom line is that you just need to be diligent about respecting any signs and symptoms that may present themselves and, of course, be sure to continue with a healthy lifestyle (i.e., no smoking or a regular steady diet of cheeseburgers!).
Kind regards,
Bill
I am a 61 year old fit female who had a SCAD 5 years ago.My arteries were crystal clear and I was told that my episode caused minimal damage to my heart and I was signed off 12 months later.I have been exercising ever since,Pilates,TRX training,spinning etc however in the last few months,since buying a polar heart rate monitor M400 I have noticed intermittent spiking especially whilst I am doing resistance work.I have no symptoms like shortness of breath or pain etc however the readings spike up to 220 + at times.I am obviously becoming anxious whilst exercising and in spite of trying different contact gel,positions of the monitor,changing monitors I still seem to get this spiking.Polar give a whole host of possible reasons but none seem to apply to my situation.Do you think this intermittent spiking is damaging my heart and/or is harmful.It seems mainly focus shed when I do exercises with my upper body.Any advice would be helpful. Many thanks, Lucia
Hi Lucia, Thank you so much for taking the time to leave a comment. First and foremost, I would strongly encourage you to speak to your cardiologist who is going to be most intimately familiar with your individual case.
If you’re 61 years old, I do think an exercising heart rate of 220+ is anomalously high and might indicate an underlying arrhythmia. I’m not saying you have an arrhythmia, but I did once work with a woman who was in her late 40s who had exercise induced atrial fibrillation. She was very fit and was a regular exerciser. She found out about it because her heart rate monitor was showing large temporary spikes in heart rate during exercise.
It’s hard to say if these spikes in HR are dangerous to you, but I can say with reasonable confidence that you should speak to your cardiologist and have further work-up as necessary. They may do a treadmill stress test in order to try and induce the same spike in HR and capture it on an electrocardiogram. They might also put you on a holter monitor in order to see what is happening when you’re not exercising.
Feel free to come back to this page and leave another comment after you’ve seen your doctor. The comments are very helpful for other readers too.
Hope this helps.
Warm regards,
Bill
Hi, this is really nice to have a person like you for guidance. I had a heart attack on 6th feb,2016, a myocardial infarction in the anterior wall with stenting in the LAD and an initial ejection fraction of 35 percent. I am writing down what i could grasp after discussion with my doctor. Please guide me as to when should i start exercise and what kind of exercise i can do. Unfortunately, i dont have any rehabilitation centre near to my town.
Hi Paro,
Thank you for your comment. First things first, if your heart attack was only 10 days ago, then you need to remember you have some healing to do before you get back to structured exercise where you’re pushing yourself. If you have an ejection fraction of 35% after your heart attack, then it is likely you had a bit of damage to your heart wall muscle. Without knowing your entire medical history, I can’t give you any specific guidelines, but I would strongly recommend that you work closely with your cardiologist and together you can determine a date when you will be medically stable enough to get back to doing more strenuous exercise.
I would suggest you read my other article on angioplasty/stent found at: https://drbillsukala.com/exercise-after-angioplasty-stent/ This article will also give you some guidelines as to what you can do in the recovery phase before you get back to doing any strenuous exercise. At this point, I would recommend that you just focus on low level walking on flat surfaces. No walking up steep hills or climbing multiple flights of stairs. Again, bottom line is that you will need to work closely with your cardiologist to determine when you can get back to exercise and how hard. Ask your doctor about having a treadmill stress test performed when the time is right.
Hope this helps.
Kind regards,
Bill
Hi Dr. Bill,
My name is Sherri and I live near Cabo San Lucas in Mexico. I just had a heart attack on March sixth and stents placed on the sixth. My Dr. Has given me the ok to walk on the beach a half hour every day. After reading about restenosis I’m a little concerned this could be too much to soon. I love it but does my heart. I’m actually not totally confident in my Dr. As he said I would go home with a monitor and do a stress test before the stents were placed. he also said he would see me weekly for a month and now as of my first follow up does not want to see me for a month. Am I just freaking out or do you think I have legitimate concerns? If you think they are legitimate could you recommend how much I should be doing until I can find another Dr.
Oh, I’m 52, fit and healthy. Not heart attack was a total surprise to my regular Drs. Only one borderline high cholesterol reading they thought was due to menopause. My cholesterol readings were back down the morning of the heart attack . This is why I think he may be so lax with me. Not sure
Thank you for your help
Sincerely
Sherri
Hi Sherri,
Thank you for your message. I certainly understand your concern and anxiety regarding getting back to exercise after a heart attack and stents.
Every cardiologist is different, but in my experience, it is quite common for the cardiologist to see you at the time of discharge and then again about 3 to 4 weeks post discharge. Unless you are experiencing overt signs or symptoms that something is wrong, there’s not much need for you to be seen every week.
Regarding exercise, if you’re walking on the beach, then this is a “step in the right direction” (pun intended). While you’re still quite fresh out of your surgery, you do have to remember that there is healing happening on the inside. From an exercise physiologist’s perspective, we want to see you exercising but not so hard that your heart rate and blood pressure are blasting into orbit (i.e., exercising at very high intensities).
Pay attention to any signs or symptoms that could mean something is going wrong (i.e., pain, pressure, or other discomfort in your chest, back, neck, arm, jaw. Shortness of breath, early fatigue). If any of these rear their ugly heads, then get to the hospital.
Sometimes the worst of this immediate post-op phase is the anxiety associated with everything that’s just gone down. I would recommend finding someone around Cabo that runs mindfulness classes (i.e., meditation). That will help you calm your racing mind.
The bottom line: low level walking will likely be more helpful than harmful. I hope you found this reassuring.
Kind regards,
Bill
My name is Michele and I am a personal trainer! Just recently at the gym I work at I have been talking to a few clients who have been referred to me with a history of heart defects!
I think because I currently train a few clients who have heart stents fitted anyone with heart related issues seem to come my way!!!!
Just recently I did a consultation with a 58 year old man who had a heart attack a few years back and had a triple bypass about 4 years ago and over a period of 3 years has been fitted with 5 heart stents! He also had an operation in his neck because his carotid artery was diseased and calcified, apparently has two sort of “patches” which were inserted inside his neck to help with this!!!
He is about 21 pounds over weight, has high blood pressure and wants to lose weight! Apparently he has been cleared by his cardiologist and told to exercise! He is due to go to hospital to discuss pains in his left calf muscle which he was told heart related! He assured me he has cut down on alcohol and does not smoke anymore!!
I am confident with giving advice on diet to lose weight however I am just a little concerned as to intensity and type of training I can prescribe!
Would I be correct in thinking that cardiovascular intensity should be between 40% – 60% of his max for about 20 minutes 3-4 times a week or should I keep that lower???
Also I am a little cautious about doing any form of weight training especially overhead because of his blood pressure however I want to increase his muscle mass percentage so that we can tackle his fat weight which he is carrying too much of!!!
I want to get his heart stronger but with out causing any detrimental side effects! Your guidance would be much appreciated as I feel I am out of my depth here! This is a perfect example of “one size does not fit all”
Thank you in advance
Michele
Hi Michele,
Looking at the information you’ve presented, I think you are dealing with a higher risk client. He’s got a documented history of heart attack, bypass surgery, AND angioplasty/stent. For his carotids, it sounds like he had a carotid endarterectomy. And now he is presenting with current symptoms consistent with what sounds like peripheral vascular disease (also called peripheral arterial disease). He is probably experiencing intermittent claudication where when he goes out for a walk, he gets left calf pain. In short, I’d say you need to be very careful with this guy. He “says” he has clearance from his cardiologist, but I would suggest having him bring you written approval from the cardiologists to cover your back. I’ve had experiences of people saying they were cleared when in fact they were not.
If he is on medications that help keep his heart rate and blood pressure down (and I assume he would be), then that is a good thing. In this particular case, based on what you’ve provided, it will be important to keep him from doing the super high intensities until you have a better gauge on his full medical history. You mention he had a heart attack, but do you know if he had any damage to his heart muscle? If so, what is the condition of his left ventricle? If he has an ejection fraction of 40% or less then you’ll need to be extra careful. There is also a possibility he could have arrhythmias, so again, you’d need to really spend the time getting into his medical history.
If he’s on beta-blockers then any prediction equations for an exercising heart rate will not be very useful since beta-blockers will lower his resting and exercise HR and BP. In that case, stick to rating of perceived exertion, around 11 to 13 on a Borg 6-20 scale.
Moving forward, I’d suggest the following:
1) Get written consent for exercise from his cardiologist (i.e., is he medically stable). Or see if he’s had a stress test at the doc’s office.
2) Get a full detailed medical history on him (ideally have him bring copies of his hospital reports)
3) Investigate which medications he is on and what effects they have on his HR and BP response with exercise
4) Make sure he gets his left calf evaluated and treated.
5) Take his resting, exercise, and recovery blood pressure during each session to establish a baseline or habitual response to exercise. People tend to hover around the same BP over time, but if you get something out of character, you can flag it (i.e., he’s usually 130/80 when he arrives and then one day he’s 200/110 = red flag = no exercise that day).
6) Make sure he gets a warm up each session and doesn’t go into exercise cold.
7) Weight training – yes, I agree it’s important not to flog him and have him doing heavy lifting. Remember that any sharp spike in blood pressure could plausibly cause a plaque to rupture.
8) Monitor him for signs and symptoms each session. Ask him about his previous symptoms because sometimes people experience similar symptoms with future events too. Look for atypical pain such as back pain which can sometimes be associated with the heart.
Bottom line on this guy: Make sure he’s medically stable and spend some time easing him into exercise. As you get comfortable with his particular condition and how he responds to exercise, you can both work together to help get him the best possible results. Hope this helps.
Kind regards,
Bill
Hi Dr Sukala,
Excellent article…..Thank you. Of particular interest is the intensity discussion. I had an MI last January. I was 47, pretty fit, normal bloods and I typically ran about 40km per week and cycled about 100km per week. I was normal BMI range. I used to exercise at pretty extreme intensity. I’ve now brought it down a lot, although I am taking metoprolol as one of my drug cocktails. I used to race competitively and I find it very hard, even now to exercise at low intensity. I have been advised by my cardiologist that exercising hard is not a smart approach. With metoprolol on board I’m at about HRmax of 145bpm and without I’m pushing 190’s. Is it accurate that exercising at high intensity has the potential to dislodge plaque with risk of this then settling somewhere and resulting in another blockage. I have a single cardiac stent. My main exercise at the moment is cycling a mix of hill and flats averaging around 30km/h for anything between 30-60 mins. Any thoughts on managing this mindset of mine and real life risks would be much appreciated. Thank you. Cheers…..AW
Hi Andrew, my apologies for the delay in responding. Your comment somehow ended up in the sin bin. I’ve rescued it from purgatory and am responding now. Technically, yes it is theoretically possible that high intensities could cause a plaque rupture provided there are other known blockages to your doctors. Everyone is different and there are some people with plaques that are more or less stable than someone else. In your case, from an exercise physiologist’s perspective, I would suggest speaking to your doc about your particular condition and whether or not you have other known blockages, what percentage the blockages are, and perhaps consider a stress test to determine if there are any abnormalities in your tracing or myocardial ischaemia. The reality is, you’re in a better place now that you’ve cast some light on the devil lurking below. There are lots of people with underlying disease who don’t know it yet and they are far worse off. The other thing is that you are quite fit and your peripheral conditioning actually compensates and takes pressure off the heart. And people who exercise often tend to have lower blood pressure responses than those who do not exercise. The bottom line is that there are always going to be risks, but comparatively the more fit and healthy you are, the lower your risk of cardiac events. Speak with your doc about your known blockages, a stress test with particular attention paid to your HR and BP response. Hope this provides you a bit of insight.
Kind regards,
Bill
Hi Bill,
I recently (31st August) had LAD and RCA stents fitted after two episodes of sharp, but not debilitating chest pain while training moderately hard on the bike. I’d experienced this maybe 3 or 4 times over the past 6 months or so, but just dismissed these incidents as one-offs, since the chest “pain” felt sort of like breathing very cold air…..it was middle of winter after all, and the symptoms disappeared as quickly as the came.
The only reason I went to medical centre this time was that I had associated forearm “pain”, well not really pain, more like an irritated, ache, sort of like “restless legs”…..and not radiating down arms, shoulders, neck or jaw…..just isolated to both forearms.
ECG at medical centre showed Wellens Syndrome pattern, so I was asked to go straight to local hospital where I was admitted.
Troponin I levels were 332ng/L, so I was shunted off to another hospital where the two stents were fitted.
Foolishly, I started back on the bike within a couple of days….VERY easy for the first three days, then the fourth day with several short (1-2min) periods where HR crept up to mid 140bpm. The rest of the time I kept it to <120bpm. All the time, during every ride, as well as before and after the incident that caused me to seek treatment, I experienced no other symptoms….no pain anywhere, no dizziness, no shortness of breath. In fact, after the incident, I rode easy for another 45min or so, went home, showered, ate lunch, then went and did a few jobs before going to medical centre….all the time feeling "right as rain"
In hindsight, I should have waited longer (3-4 weeks?) to allow better healing before doing anything more active than walking, but let's put it down to youthful exuberance (I'm 62 years young after all)
In the early hours following the fourth day of riding (6th day after stents), I woke and noticed that whenever I rolled over in bed, there would be what felt like a blood pressure cuff on my right forearm (stent was fitted through right radius) that lasted around 8-10 seconds, and then would subside and disappear. This cycle happened repeatedly….ONLY when I rolled over, followed by pressure feeling, which then disappeared.
So that morning, I returned to hospital to ask about this. During my examination, ECG and Troponin I levels of 1,450ng/L indicated a "heart attack" of minor nature had occurred………but I felt absolutely fine throughout all of this…..felt no symptoms at all, at any stage, except for this right forearm pressure that I could produce at will by rolling over in bed.
Another Angiogram to check for blockages revealed nothing, so discharged with explicit instructions from Cardiologist of NO RIDING FOR THREE MONTHS.
The Cardiac surgeon who actually fitted the stents spoke to me directly after the procedure, and said, "take a couple of days to let the insertion site heal, then you can start back very easy on the bike"
So who am I going to take notice of when getting 180 degree polar opposite advice?????
Yep, I know I should have used a bit more sense and not done so much so soon….bit I can't undo that now.
So…..bearing in mind that I'm a life-time athlete (running/cycling) and still competing at National and International level (Masters of course), in fact raced a National Championship only 10 days before my episode…..train an average 12-14hrs per week, race regularly, resting HR ~42bpm, recent Max HR 176bpm (in training) and 10-12% body fat at 63kg……can you take a swing at a few questions for me please?
1) Could my doing too much, so soon after the episode and stents, sort of "stirred up" the recently damaged heart muscle and elevated Troponin I to the ~1,450 level, WITHOUT me having had another "heart attack"?
2) Would waiting another couple of weeks from now before getting back on the bike be enough time for sufficient and appropriate healing of stent site and any damaged cardiac tissue to have taken place? That would make it 4 weeks since the stent job. I could stretch that another couple of weeks if I really HAVE to.
3) Would an arbitrary HR ceiling of something like 120bpm (mentioned in your broad exercise advice after heart attack) be within reason? I'm currently walking a couple of times every day wearing a HR Monitor to see what's going on, and easy to moderately fast walking sees my HR at 65-75bpm.
4) And the big one……is there a chance of me returning to competition in the future? I'm in no hurry….as long as I make it back to racing.
Sorry for the huge ramble here Bill………go to say, everything I've ever read in your articles and advice is understandable and logical, without "soft-pedalling BS"….and to me at least, and I've always found that to be an excellent guide to the worthiness of advice.
Thank you for your ongoing commitment to making sensible advice readily available to your many readers. It's always reassuring to have someone offer solutions instead of saying "your life is over".
Cheers,
Allan
Hi Allan,
In answer to your questions:
Q1: After an angioplasty/stent procedure, you do need some time to simply let everything settle down and heal. Even if you feel great, you have to understand there is still healing happening on the inside. It’s tough to say exactly what happened to you and we simply do not know if your elevated troponin was cause and effect from the post-stent exercise or if it just happened to occur at the same time (bad timing).
I would suggest speaking to your cardiologist and discussing if having an echocardiogram is appropriate for you to determine if you had any significant heart muscle damage and if it has resulted in any wall motion abnormalities.
As for the recommendation to not exercise hard for 3 months, I cannot provide any information here that directly contravenes your doctor’s advice (since that is both illegal and unprofessional). I can corroborate the fact that you do need to cool your jets after having what is still a heart operation (even if they didn’t slice you down the middle and do a bypass procedure on you). It may be in your best interest to seek out a cardiac rehabilitation program near you that could allow you to exercise whilst wearing a telemetry ECG unit. Taking it one step further, you might also consider speaking with your cardiologist about having a treadmill stress test to see how your ticker fares at very high intensities consistent with what might occur while you’re training and/or competing. This will give you an indication if there are any underlying issues you need to bear in mind.
Q2: You asked: “Would waiting another couple of weeks from now before getting back on the bike be enough time for sufficient and appropriate healing of stent site and any damaged cardiac tissue to have taken place? That would make it 4 weeks since the stent job. I could stretch that another couple of weeks if I really HAVE to.”
Allan, I’ll humorously say that you’re a difficult patient! So am I! When I’m injured, the first thing that goes through my mind is when can I get back out there on my surfboard! I’ve surfed with blown knees, broken ribs, and darn near a broken neck. BUT, having said that, I honestly can’t answer those questions since I’d pretty much be practicing medicine without a license. I’m a PhD-level exercise physiologist, not a cardiologist. Even if you don’t like it, you’ll still have to abide by your cardiologist’s recommendations. Again, I’d suggest joining a cardiac rehab program to put you on the right track as safely as possible. Your doc would probably agree with this.
Q3: You asked: “Would an arbitrary HR ceiling of something like 120bpm (mentioned in your broad exercise advice after heart attack) be within reason? I’m currently walking a couple of times every day wearing a HR Monitor to see what’s going on, and easy to moderately fast walking sees my HR at 65-75bpm.
This is an excellent question but even as an exercise physiologist who’s worked with more cardiac patients than I can count over the years, I can tell you that each and every person is different due to the nature of the heart disease, procedure performed, medications prescribed, and many other factors. There is no cookie cutter rule for this, but if you do participate in a cardiac rehab program, then you will work all this out with them (make sure they have an exercise physiologist on site with at least a master’s degree in Ex Phys).
Q4: You asked “And the big one……is there a chance of me returning to competition in the future?”
I’ve worked with quite a few people who, after their heart attack and/or angioplasty/stent, have managed to go back to competing at a high level. BUT, it really does depend on the individual and, since I’m not your cardiologist who knows all about your situation, I can’t give you a green light here. If you manage to get a maximum effort on the treadmill stress test and your doc does not see anything out of the ordinary, then he might give you the go ahead to get back to training/competing at a high level.
Hope this helps,
Bill
Hello Dr Bill.
on 5th of aug 2016, i had a MI with full blockage of LAD. Was unexpected as i am 39 yrs, no history of BP, Cholestrol, etc. Prior to MI, i was a regular mid-level badminton player and played for an hour, 4-5 days of a week. Main issue being smoking. The MI started in a very hollywood style with heavy chest pain, cold sweat, feeling of nausea and weakness in knees. Was rushed to Emergency of a close-by hospital (Sakra World Hispital), would have taken about 50 mins to reach there. After initial check was rushed for angiogram which resulted in angioplasty of LAD with a single DES stent. according to doctor, there was damage to heart muscle. The EF during the precedure has dropped to 20 and BP had drastically dropped. was in CCU for 4 days and was relived from hospital on the 5th day. Doc had advised light walk for the next 3 weeks. Post 3 week the EF was at 35% on the echo, and at the 6th week visit, the EF had improved to 40% and doctor advised to increase the walk from normal to brisk and to do it for about 45 mins in a day. i have been doing that without any difficulty. infact hve started mixing a bit of light joggin with my brisk walk sessions hope that is not a issue. I have been personally feeling fine in the upper body but light pain and wekness feeling is there in both the knees. could this be related to all the usual medicines? Also, i wanted to ask that when would it be safe to start riding my mid-weight motorcycle (weighs about 160 kgs)? I need to start to get back to my work and motorcycle is almost the only peoper way of commuting to my work place. Thanks in advance.
Hi Nasir,
Thanks for your comment. I would suggest the following:
1) Speak to your cardiologist about having a treadmill stress test done. If you can tolerate reasonably high workloads and the doc does not see any abnormalities on the ECG or your heart rate or blood pressure responses, then that’s a good sign.
2) Regarding riding your motorcycle, I would discuss this with your doctor to get the final clearance. I’ve had patients who were able to get back to riding their motorcycles after a heart attack, but each person is different so it’s important to get clearance from your cardiologist.
3) It’s hard to say if your symptoms are related to your medications, but there can sometimes be side effects. If these are concerning you, I would suggest speaking to your cardiologist about other alternatives that may have fewer side effects.
Hope this helps.
Bill
Hi Dr Bill!
My dad had a heart attack 2 days ago, he’s feeling better but can’t get up on his own, his heart rate has been between 60 to 95 and saturation is between 92 to 98 with out oxygen pump. His echocardiography was normal and wasn’t concerning. Tomorrow is his angiography and I hope it will bring good news too
I was wondering why hasn’t he been able get up on his own, do we need to be concerned?
Hi Shehroz,
Thank you for your comment. I am hopeful that your father is doing well after his angiography. I would also imagine they have a better idea of the condition of his arteries and the level of blockages. Perhaps they did an angioplasty as well (?). I’m not certain as to why your father has not been able to get up on his own, but one thing I can tell you is that for some people, a heart attack can leave them quite tired in the immediate aftermath. I would bring this to the attention of his doctors as they will be most familiar with his medical history and can provide you with a more clear explanation. Best wishes to you and your father.
Hi Dr Bill! Sorry I was very busy and I just read your comment.
Yes my dad had an angioplasty and his angiography revealed a 2 artery problem and the doc said he only needs one stent. He’s back to work now after 3 weeks rest. His doc cleared him for salt and stairs too
Dr. SUKALA
Firstly I would like to thank you for this informative article. I’ve just discovered you and can’t wait to read more of your work. Secondly, understand it is hard for you to offer actual advice to someone you do not know so I will ask as a general question.
If someone is in their 20-30s and exercises regularly, with no congenital birth defects or family history for things such as aneurysms, aortic or in the brain. And if that person were to go to a neurologist and cardiologist get ct scans, ekg, echo cardiograms etc all of which came back negative and told they are at this point a perfectly healthy adult, to which degree if any is strenuous weight lifting/ cardio a danger to their health.
Instances of healthy individuals dropping dead from such things is documented although I believe to be rare. However, as a health enthusiast I lift and exercise to increase my longevity and quality of life. What do you tell to a young healthy athlete with no conditions who has had testing done. Also, in what way do things such as PVCs relate to this (the reason I got the work ups done in the first place) I was told it could be athletes heart and it was completely benign.
Thank you so much in advance for the help.
Hi Vincent,
Thanks for visiting my site. I’m hopeful you’ve found a few helpful bits to move you along in the right direction. You’re correct in that I can’t offer any specific individual advice, but I can certainly provide a few considerations you might wish to discuss with your doctor.
First off, the occasional PVC is common and, for the most part, if there is no underlying disease precipitating them, then the docs usually dismiss them as benign athlete’s heart (as you rightfully pointed out). It’s still smart to get them checked out just in case, so kudos to you for that.
Given all the other information you’ve provided, that your scans came back clear and you’re a regular exerciser, then all you would need to do is get final clearance from your cardiologist to get back into the gym.
I think it’s important to remember that exercise is a challenge to the body. And as such, there are risks involved whether you’re perfectly healthy or have had medical issues. So from an exercise physiologist’s perspective, I’m all about minimising risk and maximising safety. If I had someone come to me in your situation, I would check that all the tests had been done and that you had a signed clearance to exercise. I would then start off at a moderate intensity with sign and symptom monitoring (heart rate, blood pressure, shortness of breath, any feelings of palpitations in the chest, etc). If that all came back clear, then I’d gradually work to higher intensities. If symptoms reappeared with exercise and were worrisome (i.e., palpitations in the chest for an extended period of time), then I’d contact my doc again and see what he/she thinks would be a prudent course of action.
The occasional PVC or two isn’t much of a concern for the most part (especially with tests all clear), but if they become sustained then that’s a whole separate cause for concern.
Bottom line: get clearance from your doc and then ease back into your exercise but just be more aware of any signs/symptoms than you previously were. The reality is, most people don’t just drop dead (that is rare). They often have signs and symptoms they ignore but didn’t tell anyone.
Hope this helps.
Cheers,
Bill
Hi Bill,
I’ve wrote before after a heart attack Nov 15, i had 1 stent put in the widowmaker artery & no heart damage, I’m now 57. I attended cardio rehab done well & resumed my squash plus running march 16. In Dec 16, I had a bad day went to hospital they kept me in for 2 nights for observation, the cardiologist confirmed it wasn’t a heart attack or angina, when I mentioned squash he said it would not cause a heart attack.
They recommended an angioplasty which was performed Jan 17, another 3 stents were placed in, I’ve been good since then. I didn’t take up the offer of cardio rehab this time, now I’m thinking of playing squash and jogging again. Would 4 stents have a big difference or would I be more fitter now that the plumbing is evened out.
My feelings are I should be happy just going walks as the NHS medical services in the UK have been excellent giving me these extra days and don’t want to jeapordise this. I just miss the competitive edge a team game of squash gives but I will give it up if needs must.
I read other people’s questions and your replys which is very interesting, thanks for taking the time.
Hi Tom,
Thanks for your comment. Everyone is a little different of course, but theoretically, if you’ve had more stents placed and they are working well, then you should have no blood flow restrictions to your heart and be able to resume your usual activities. BUT, having said that, I always urge people to speak to their cardiologist in depth about their specific circumstances. Nobody but your cardiologist and direct medical management team can give you more specific and guided direction than them. Also, the fact that you did NOT have any damage to your heart muscle is a good thing. If you had damage to the myocardium then that would potentially change the playing field a bit. Bottom line: I’d suggest 1) speaking to your doc about your condition and your desired level of exercise intensity; and 2) perhaps seek out a qualified clinical exercise physiologist who can liaise with your medical management team and perhaps put you through the paces with an ECG to see that all the blips and squiggles are normal! Hope this helps. Cheers, Bill
I am just 32 years old having serious heart attack. I had done bypass surgery. I have also scoliosis on my back. My heart is working at only 55%. After one year of bypass surgery I still have muscle pain. But my doctor say it will goes away. I had pass treadmill test. My doctor says now you are alright and do want everything you want. You can climb hills without any fear. But I am very depressed. I always feel fear.
Dr. Bill please tell me my physical limitations? What is my life expectancy?
Hi Azhar,
Thank you very much for taking the time to leave a comment. First, it is not uncommon (even normal) to feel depressed and have fear (anxiety) after a heart attack and bypass surgery. Having heart problems is a scary experience and you don’t have to try and “be strong” and deny those feelings. I would strongly suggest speaking to a counsellor or social worker at your hospital or clinic to discuss your feelings. They can help you work through this and help you find some peace of mind.
Second, if your ejection fraction is 55%, then you’re actually doing quite well. This does not indicate severe damage so that is a VERY good sign. You can read more on ejection fraction here: http://www.mayoclinic.org/ejection-fraction/expert-answers/faq-20058286.
Third, as for your pain, I can’t actually say for sure when this will go away since everyone responds differently through the recovery period. But remember that open heart surgery is hard on the body and it DOES take time to heal.
Fourth, if you’ve had a max treadmill stress test and you passed, then this is a good sign as well. If you are climbing hills at an intensity less than what you experienced during your treadmill test then you, should be able to safely tolerate that level of exercise.
Finally, as for your physical limitations and life expectancy, I can’t really say for sure since I am not familiar with your entire medical history and have not worked with you. Your best bet is to discuss these questions with your doctor who will be able to give you a more thorough answer. But as I said in the beginning, I would strongly advise you to speak with a counsellor/psychologist/social worker who can help you work through these feelings. Rest assured they are very normal feelings given all you’ve been through. Feel free to stop back and leave another comment after you’ve spoken to your doctor and/or a counsellor.
Kind regards,
Bill
4 years ago I suffered From “the widow maker” while I was at crossfit. I did not know I was having a heart attack . I thought I was just suffering through the hardest workout of my life. The next day about 20 hours later I went to the ER and was admitted and had a stent placed. I have some scar tissue on my heart now and my cardiologist advised against strenuous weight lifting. But said I could do light weights at high reps to keep my blood pressure low as to not strain / stretch the damaged tissue in my heart.
I miss lifting heavy weights and find high rep weight lifting just boring.
What are your thought about heavy lifting and scAr tissue on the heart. Will it really stretch out and tear causing me to bleed out internally?
Is there any safe way to lift weights ?
My cardio is pretty good and about where it was before.
I’m only 44 and want to get back in shape.
Hi Josh,
Thanks for your comment. There are a few things to consider here:
1) How big was your heart attack? Did the docs give you any indication of your troponin levels?
2) Do you know what your ejection fraction is now 4 years after the heart attack?
3) Have you done a max treadmill stress test recently? If so, what was your max heart rate and blood pressure response?
4) Do you currently have any chronic ventricular arrhythmias stemming from the heart attack/scar tissue?
5) Do you have high blood pressure? Or did you at that time? Are you currently taking medications to control your BP?
6) Was your heart attack due to coronary artery disease or did you have a one-off out of character vasospasm in your artery that made it clamp up in that instant? The latter is not common, but I’ve seen it happen from time to time. You seem quite young even if this happened at 40.
The reason I ask these questions (from an exercise physiologist perspective) is to get a gauge on how much damage was done to your heart and how that is affecting your heart’s ability to pump blood to your body (ejection fraction).
If you had a max treadmill stress test and were able to tolerate high workloads without any rate or rhythm abnormalities (arrhythmias) and your blood pressure response was linear with exercise intensity but was not astronomically high (i.e., 300+/110+), then that is a good sign that you can do higher intensity exercise (with clearance from your cardiologist).
If you have any underlying ventricular arrhythmias like runs of ventricular tachycardia then that is something that would likely raise your doc’s eyebrows. But if you’re in normal sinus rhythm at rest, during exercise, and afterwards in recovery, then that would give me a warm fuzzy feeling inside.
Finally, if your blood pressure is within normal limits with or without meds and you do not have any other significant cardiovascular risk factors, then that could help bolster your case when you talk to your doctor.
The bottom line is that you’re just minimising risk, but you can’t eliminate it (whether you’ve had a heart attack or not). Exercise by its very nature carries risk, and even if you do everything right, sometimes bad sh*t happens to good people. I would suggest that you speak to your doctor and work together to discuss these questions I’ve presented above and, when viewed through your specific medical history, can you minimise risk enough that you can return to heavier (heavy) lifting (even if it’s not Crossfit)? I can’t legally give you any concrete yes or no answer here since I’m an exercise physiologist and not a cardiologist, but I can tell you I have had patients come through the cardiac rehab program that went back to lifting reasonably heavy weights even in their 60s, 70s, and 80s. But again, it is different from person to person and depends on a multitude of factors. Remember that if you get the approval from your cardiologist to go back to lifting heavier weights, there are going to be risks, but if you minimise those risks as much as possible, then chances are you’ll probably be ok.
Hope this helps.
Bill
Thanks for the reply.
My EF is about 50%
I have had a treadmill test and the results were good. I don’t know the specifics but my Dr. Seemed happy with them. I currently mountain bike and use the row machine ant decent paces. (5k in 25min)
No chronic arrhythmias
I did not and do not have High BP OR any other risk factors like high cholesterol or any genetic factors.
I was told it was just bad luck.
I am on low Dosage meds Coreg , Lipitor, atorvastin , aspirin.
And take magnesium citrate
My heart attack was caused by a small pocket of new plaque that ruptured.
In the imageing my arteries looked to be in normal condition and no other sign of heart disease or excessive plaque build up.
I’m
Not sure of what my triponin levels were. But I do know there was heart damage because I waited so long to go in. Dr. Told me the reason I didn’t just drop dead on the spot was because of my excersize habits and my heart had built up collateral circulation. So I feel like excersize saved my life and I want to be back in good shape in case this happens again. I did take my bp monitor with me to lift weights once to see how big it went during the lifting. My bp Went close to 200 over something.
I wonder how high my bp would need to be to cause damage.
Thanks for the guidance. I need to talk more with my Dr. And see what his real opinion is about my specific case.
Hi Josh, thanks for your comment. Yep, I assumed it was one of those one off anomalous heart attacks. Based on the info you’ve provided, I think you could probably make a compelling case to your doc to start lifting weights at higher intensities. Max lifts or sustained maximal efforts might still be unadvisable though due to the potential for astronomical spikes in blood pressure, but I’ll leave that to your doc’s discretion. Also, your EF% is 50% so considering all that happened to you, you are quite lucky it’s still that high. I think I’d focus on asking your doc about the scar tissue and how that might respond to high intensity resistance training. Ask him if there is any cardioechographic evidence of any wall motion abnormalities. If your heart is otherwise functioning well and your BP is under control, which it sounds like it is, then he might give you the green light. Good luck. Cheers, Bill
Is there correlation between LVEF and max heart rate possible ?
Hi Carlos,
If you have a reduced LVEF after a heart attack, depending on the extent of heart muscle damage and its effects on your EF, the heart rate may increase to try and meet oxygen needs of your body’s organs and muscles. In some cases, there might also be irregular heart rhythms (arrhythmias) as in after a heart attack. So your standard max heart rate may not be relevant if there are extenuating circumstances such as a heart attack and reduced LVEF. The best person to consult is your own cardiologist who will be most familiar with your particular medical history. Hope this answers your questions.
Kind regards,
Bill
Hi Dr. Bill
Thanks for your article and responses. They are what I’ve been looking for. I am particularly interested in the responses you gave Josh above. I’m 57 had a STEMI related to ruptured plaque. I had been having intermittent resting chest pain in the afternoon which I assumed was the blood clot forming but not fully blocking off the artery. MI occurred in the evening in the hospital but was at the top of the artery (anterior wall). They couldn’t catch the abnormality on the EKG until it fully blocked. Troponins were 200. All this took placed in May 2018. Was previously diagnosed with CAD but calcium score was 77. Inherited risks and had been on statins for 15 years.
Before the MI I was doing high intensity cardio with heart rate in the upper 140’s and hiking 4-6 miles in the mountains around my house regularly.
I’m on 6.25 mg Coreg, 90 mg Brilinta 80 mg Lipitor and 10 mg Zetia and 81 mg aspirin. Resting BP 115/75 on average. If i take ACE or ARB I’m exhausted because my BP drops too low. My LVEF has been holding steady at 45-50. no known arrhythmia.
I did cardiac rehab and they let me go because everything looked fine. Cardio is supposed to be less than 130 BPM. I started 30 reps of weight training after cardiac rehab with core exercises (w/out weights) and have been doing for about 4 months twice a week. I live at ~6000 ft elevation.
If I push a little too hard on either hiking or on just a little bit more weight I get exhausted later in the evening and the next day. My chest feels heavy and tired. I’m not really sure when I’m doing something if I’m pushing too much. Sometimes if I haven’t gotten a good night’s sleep and I exercise at regular intensity, I will get really tired afterward. In other words it’s hard to define my limits.
My cardiologist is no help, so I’m trying to understand if I just have to learn my limits better or if I’m doing something wrong/damaging my heart. To me there seems to be variables that don’t seem to explain why I get so tired.
Any thoughts or input would be helpful.
Thank you so much for this page.
Hi Glenn, thanks for your comment. It sounds like there are a lot of moving parts at work here so it’s hard to narrow it down to any one thing. On a positive note, your LVEF seems to be pretty good. Medications can really knock you about, so sometimes even if you feel motivated to get out there on the mountains and attack, you may feel like you’re not able to give it your all. As I’ve said in other responses, I’m no fan of pharmaceutical meds, but in the case of heart attacks and preventing future events, sometimes it’s a case of “better the devil you know than the one you don’t.” The Coreg in particular might knock you down a few pegs. Overall, you’ve ticked all the right boxes and you appear to be medically stable based on what you’ve written (you’ve been to cardiac rehab and presumably you’ve got clearance from your cardiologist to get back into reasonably strenuous activity again). If you have your heart rate limits that were set at the cardiac rehab program, then it may just be a case of doing some trial and error and finding the exercises and intensities which best suit you. Also consider the diet side of things too, ensuring that you’re getting adequate nutrition to fuel your exercise both in terms of meals and during exercise (particularly during long duration higher intensity activities like hiking). Hope this helps. Kind regards, Bill
You made a great point when you stressed the importance of going to cardiac rehab after a heart attack. My dad recently suffered a heart attack, but currently has no plans for rehabilitation. Like you pointed out here, they can help him improve his lifestyle and tell him how to exercise safely. I will see if I can convince him to find a cardiac rehab facility he can visit.
Definitely have him attend cardiac rehab. He’ll be glad he did.
Hello Dr Sukala
My husband had a quadruple bypass at 46 years of age. Then he had a cardiac arrest in 2016 at 65yrs of age. He has always been stubborn about listen to Doctors, Cardiac Rehab nurses,Specialists at RNS Hospital. He has always walked that’s how we found out about him having the bypass. He has been told to slow down but since his cardiac arrest he still didn’t listen and has gone on to bush walking by himself up to 3 hours at a time, doing 22,000 plus sometimes more and it’s everyday. We split up due to his aggressive behaviour which he didn’t have before plus his exercising plus more. He still drinks but has cut down, and he has lost weight. Can you tell me if it is alright to be doing this walking? Also he has a Sewing Machine Business and he works 5 half days.
Hi Christine,
Yeah, sometimes the one thing they can’t cut out of them in surgery is their own stubbornness. It’s hard to say what’s going on, but at a glance, he might be in denial which is the first stage of the grief process. Having major medical issues can really get into someone’s head and cause them to grieve the metaphorical “death” of their previous healthy selves. The stages of grief are D.A.B.D.A (Denial, Anger, Bargaining, Depression, and Acceptance). Noting that he is also being aggressive could plausibly be related to the second stage (anger).
In relation to his exercise volume, if he is deemed medically stable and is not having any signs or symptoms, then exercise might be the very thing keeping him alive and protecting him against future cardiac events.
Depending on your current relationship with him and if he’s willing to listen, it would be wise for him to speak to a counsellor with experience in helping people with major medical issues. If he is experiencing significant loss of his former self, then he would benefit from being able to speak to someone to help get some perspective on things.
Bottom line: only he can help himself and it’s unfortunate that there is some collateral damage to his personal relationships as a result of his aggressive behaviour. If you or someone else in the family can get him to be honest with himself and encourage him to speak to a counsellor, it may very well help him find a sense of grounding. Feel free to stop back with an update if you’d like. It’s helpful for others to read these stories as it may help them in their recovery process.
Kind regards,
Bill
Hi Doctor,
It has been 3 years since my heart attack . Last December I had my last check up and result are relatively good. My LVEF is still below 35 measured by ultrasound). Although I feel good My doctor recommend implanting ICD.
I am 66 yo. Do I have to go for it or there is still something could be done in order to improve my LVEF?
it looks like that there is line of LVEF of 35%. below that is advisable to have it.
Can I have your thought please?
Thank you
Hi Georgi, Thanks for your comment. Your left ventricular ejection fraction (LVEF) is only one piece of the puzzle. Remember that even if your LVEF doesn’t change much, if you’re doing regular exercise, there will be adaptations in the rest of your body that will compensate and protect your heart. Exercise changes the physiology and biochemistry of your body in ways that benefit your heart. For example, your muscles become more fit and efficient at extracting oxygen and nutrients from the blood. So for every heart beat, the rest of your body is working more efficiently.
As for improving your LVEF, you’ll have to speak to your doctors about this. It can be different for each person. Since your heart attack happened three years ago, your LVEF might be stable now. The real question is whether or not it’s stable. Hopefully it’s not getting worse. That should be a bigger concern. But bottom line, remember that regular exercise can help your overall body work more efficiently. Hope this helps.
Kind regards,
Bill
Hi Bill. Thanks for the reply. I took your advice regarding medications limiting heart rates and backed off. Moderating my exercise helped a lot. My stamina increased significantly and I was able to increase my intensity somewhat. Its been > year since my MI and I’ve worked with my cardiologist and am only taking Zetia and Atorvastin. I didn’t have high blood pressure before and don’t have it now that I’m off Coreg. The fatigue is gone and no chest pain or shortness of breath caused by Brilinta. LVEF is now around 55. My heart rate increases more when I hike, exercise, lift weights, etc. Coreg had kept it at 120 to 135 and I can easily go up to 150 bpm when I’m hiking a mountain. I have an Apple watch for the express purpose of monitoring my heart rate. This allows me to increase exercise intensity more but I’m not sure where I should limit my heart rate. Are there general guidelines that have been established to calculate heart rate limits after a heart attack? The rates they established during rehab are really low intensity and don’t seem meet my needs for exercise.
I really appreciate your help. Reading your articles and responses to my and others comments helped out a lot
Thank again, Glenn
G’day Glenn,
Thanks for taking the time to stop back and leave a follow-up comment. Nice to have some feedback.
In the immediate post-heart attack phase, yes, the heart rate guidelines are quite conservative as follows:
Post-MI: Maintain heart rate (Hr) less than 120 beats/min or heart rate at rest + 20 beats/min
However, once you’ve been through the initial cardiac rehab and assuming you are medically stable and cleared for higher intensities by your doctor, then you probably won’t have too much to worry about. As I may have said in a previous response, for those who are quite active, I often recommend asking your doc if you can have a treadmill stress test performed to see how your heart goes at high workloads. If you have a normal rise in heart rate and blood pressure, no cardiac arrhythmias, and no signs or symptoms (other than the expected fatigue and shortness of breath due to the high intensity), then your doc may tell you that it’s safe to get back to working out hard again.
The most prudent course of action is always the same: maintain good communication with your doc and discuss the risks vs benefits of higher intensities.
Hope this helps.
Cheers
Bill
Hi Dr Sukala,
I had a heart attack in 2016 aged 49, and had one stent fitted. While I was in hospital I found out my mother was diagnosed with breast cancer and on New Year’s Day 2017 she passed away. Having lost both of my parents close together I suffered from depression and anxiety, have led a pretty sedentary lifestyle. My mental health is much better now, but now I’m concerned about getting back into exercise after so long. Do you have any suggestions or tips for starting again? I really don’t want another heart attack.
Thank you Dr Sukala,
Pete.
Hi Pete,
Thanks for your message. I’m very sorry to hear about losing your parents and having to go through all that with your own heart. Getting back into exercise will, of course, help you physically, but it will also help your mental health as well.
The first and most important thing is making sure that your heart is stable. I’d recommend speaking to your cardiologist during your next check up and ask if there are any specific precautions relative to your medical history that could possibly cause any problems with exercise. Chances are, you’ll be ok. You might even request a stress test which will allow the doctor to see that your heart is working normally at rest, during exercise, and after exercise (i.e., normal heart rate, rhythm, blood pressure, nothing abnormal that could pose a risk). Assuming that’s all normal, then realistically, you should be able to get into exercise without any issues.
While it’s true that you had a heart attack and stent placed, it’s also true that you’re still a human being and your body works the same as anyone else’s. As a general rule, just be sure to ease into it and not try to take on too much too soon (i.e., super heavy, high intensity lifting on day one).
You might consider hiring an exercise physiologist in your area that has experience working with people who’ve had a cardiac intervention. This will probably help put your mind at ease and facilitate a safe progression.
Hope this helps.
Kind regards,
Bill
Hi Dr Sukala,
Thank you very much for your reply, it was very much appreciated.
Best wishes and thank you again,
Pete.
Hi Dr. Sukala,
Just a quick question for you. I realize you probably get a lot of messages so thank you for your time. I am 39yrs old, competitive bodybuilder who had a heart attack from a fully blocked Right Coronary Artery. Diagnosed with moderate left ventricular hypertrophy. Put on Plavix, Lisinopril, Metoprolol, aspirin, Atorvostatin. Energy-wise I felt fine/normal two days after the stent. I waited two weeks to go back to gym. Started with 15min steady walk pace. Some light ab work and started very light weights. After few sets of 15-20 reps very slow, I only noticed a very slight cramp feeling in lower chest when taking deep breath. This feeling went away after few minutes and not present with normal breathing. Same feeling one would get if running hard. My heart rate was still lower than 100. Is this expected? Did i go harder than I was ready for? Due to insurance complications, I wont see my cardiologist for two more weeks so looking for your thoughts. Thank you again! I do appreciate it.
Hi Dain,
Thanks for your comment. A few things to consider here. If you’re a bodybuilder, it’s not uncommon to have a bit of left ventricular hypertrophy. Did your doctor confirm this was due to the exercise? Or from any other pathology?
Also, was there any indication from tests that you had any damage to your heart muscle? If there is any damage to the myocardium itself, that can potentially require a bit more healing time.
In many cases, an angioplasty with stent only requires a couple days in the hospital, but full healing time can extend out to at least a month or so. In other words, even if you’re feeling good (which is a sign the stent is working), it’s important to remember that there IS still healing happening on the inside.
It’s hard to say exactly why you experienced the cramp, but I have heard of quirky things like this in some people after angioplasty and stent. But the thing to ask is, was it a cause and effect thing (meaning, did the angioplasty/stent cause the cramp) OR was it just a coincidence of two things happening at the same time but one did not cause the other (meaning, you had a cramp from exercise, but it just so happened to occur after you had an angioplasty / stent procedure)? These are the things that you’ll want to discuss with your doctor.
While you’re in the initial recovery phase, there is nothing wrong with laying low for the first month. Yes, you can still do low level exercise as long as you’re paying attention and monitoring yourself for any signs or symptoms (chest pain, shortness of breath, all the usual suspects).
Usually, a month after your procedure, you’ll have a follow up appointment with your cardiologist. Just be sure to mention these things and discuss your concerns. I can certainly appreciate that being an active individual, this sort of thing is even more psychologically worse than for someone who is a life-long couch potato. In other words, it’s a quality of life sort of thing, so be sure ask all your questions at the appointment, as your doc will be most familiar with your medical history. You should also ask if there is a practice nurse on duty at the cardiologist’s office that could be available to take your phone call if you should have any further issues. This way you don’t necessarily need to go through the hassle with insurance to get another appointment sorted out. I worked in the healthcare system in California and had to fight insurance companies nearly every day, so I can really empathise with your frustration.
Hope this information helps point you in the right direction.
Kind regards,
Bill
Dr. Sukala,
Thank you for your response. I really appreciate it. I was told roughly 13 years ago during an echo stress test that the cardiologist at the time also saw slight thickening to the left ventricle but he said he sees that often in athletes or weight trainers. The cardiologist in the hospital was not much help to be honest. He was very vague on answering questions and once his cell phone rang, he lost all attention. He didn’t get specific on damage. All he said was ” anytime you have a heart attack, theres going be damage” I also asked about blockage in other arteries and he said “yes”, but said he couldnt remember which, he’d have to ask the doc who did the stent… However, my post PC doc reviewed my whole stay in hospital and couldn’t find any notes on damage and or other blockages. The attending cardiologist post stent was not the same as who did the stent. Insurance differences has me seeing a different cardiologist all together on Sept 30th.Good news is , I trained today doubling my cardio time plus some light weight training and felt great! No cramping, no shortness of breath, etc. Did very light weights.
Im curious on your opinion to this- there’s no saying how long i had this blockage and thicker left ventricle while still training very hard before my MI, correct? I feel that since this stent has my blood flowing much better , im actually in better health now then I was for who knows how long before I had this happen…..do you agree? Do you feel the meds Im on such as blood thinners are usually a long term thing? Im assuming the bp, cholest, and beta blockers , aspirin will be…..(?)
Lastly, are you personally against someone in my position using a therapy dose of testosterone weekly?
I really appreciate your time,thoughts, and expertise! Helps keep my mind at ease to hear a second viewpoint. Again, i know not a diagnosis/medical advice but helps alot!
Dain
Hi Dain,
Thanks for your comment. I’ll try to address some of your key concerns below:
You wrote: “All he said was, ‘anytime you have a heart attack, theres going be damage’”
I think it’s more appropriate to phrase it as there is a “possibility” of having heart damage. In the cardiology world, there is an expression that goes: Time is heart muscle. In other words, the quicker you get to the hospital, the quicker they can administer clot-busters and/or do an angioplasty/stent. If you delay treatment, then yes, there is a greater likelihood of damage to the heart muscle.
When you talk to your cardiologist next, ask him what your cardiac enzyme levels were (troponin etc) and if they indicate a small, medium, or large heart attack. Also, ask if the imaging reports indicated any wall motion abnormalities. If there is damage, then this might translate to abnormal cardiac wall movements when pumping.
Also note that it’s possible to have what is called “stunned myocardium” where the heart muscle is somewhat damaged but can regain its contractile function in the recovery phase. I’ve seen this on a number of occasions.
You wrote: “I also asked about blockage in other arteries and he said “yes”, but said he couldn’t remember which. My post PC doc reviewed my whole stay in hospital and couldn’t find any notes on damage and or other blockages.”
This is good news on both accounts. If there is no damage and no other blockages, then this is a very good thing. Of course, moving forward, you will want to be proactive with getting periodic check-ups to make sure nothing else is brewing in another artery. You don’t need to be neurotic about it, but just be diligent in keeping up with your periodic appointments.
You wrote: “Good news is, I trained today doubling my cardio time plus some light weight training and felt great! No cramping, no shortness of breath”
Being young and fit is actually a very good thing that will work in your favour moving forward. People who have had cardiac issues and have a healthy lifestyle (i.e., exercise, etc) are more likely to be able to live normal healthy lives moving forward (as opposed to those that continue to smoke, eat a steady diet of cheeseburgers, and don’t exercise). Keep on doing what you’re doing. Once you see your cardiologist at the end of the month, you can ask questions about how hard you can go re: exercise intensity.
You wrote: “I’m curious on your opinion to this: there’s no saying how long i had this blockage and thicker left ventricle while still training very hard before my MI, correct?”
It’s hard to say. If your first sign of any heart trouble was this particular event, then you have no previous medical records related to it that you can evaluate. Also remember that people can develop blockages at different rates. Some accumulate over time where others, perhaps with a strong family history of cardiovascular disease, might develop blockages quicker.
Being a young person, I would also recommend that you ask your doctor if there is any indication that your heart attack was caused by a build up of plaque (lesion) or if it was a vasospasm. I have heard of cases of people who are healthy and have heart attacks due to a coronary artery spasming. It’s not common, but it’s possible. In your case, if you did have a spasm, then that is not the same thing as coronary artery disease.
You wrote: “I feel that since this stent has my blood flowing much better, I’m actually in better health now then I was for who knows how long before I had this happen…..do you agree?”
The good news is that, despite something bad happening, at least it’s better the devil you know than the one you don’t know. I’ve seen situations where a person’s first sign of heart problems was sudden death. So to that end, you had symptoms, you got treated, and at least it’s managed. Now that your stent is placed, you should be feeling better, to the extent that it was limiting you previously. Lots of blood flow to the heart certainly isn’t going to work against you. Moving forward, as I said above, it’s going to be important to keep up with your healthy lifestyle, keep your cardiologist appointments for check-ups etc. If you do all that, realistically, you will significantly minimise risk and decrease the likelihood of a second heart attack. Again, better the devil you know than the one you don’t know.
You wrote: “Do you feel the meds Im on such as blood thinners are usually a long term thing? Im assuming the bp, cholest, and beta blockers , aspirin will be…..(?)”
I honestly couldn’t give you an answer on that. Only the doc managing your condition can answer that. Though, you might want to ask your doc if it’s possible to decrease your dosages over time if it’s medically prudent to do so and, possibly, discontinue them if he/she feels the risk is low enough. I am aware that the beta blocker (metoprolol) can make some people feel quite lethargic, so if that becomes an issue, then you might want to discuss this. I’ll be the first to admit that I am NOT friend of the pharmaceutical industry, but there are times where the meds can significantly reduce your risk and may be medically warranted. Bottom line: speak to your doc who will have your medical history there and discuss these issues to your satisfaction.
You wrote: “Lastly, are you personally against someone in my position using a therapy dose of testosterone weekly?”
Again, this is something that you’ll have to discuss with your doctor. In general, I can say that it’s best NOT to screw with your hormones unless there is a DAMN GOOD medically-warranted reason for doing so. If your testosterone levels were dangerously low and it was causing problems, then perhaps that’s a good case. But I have seen all these youth/aging clinics popping up and pumping people full of testosterone and growth hormone for a few thousand dollars per month. But my concern is that once your body begins to grow dependent on them and, for whatever reason, you decide to stop, you can’t just stop. Lots of moving parts to the story, but ultimately, in your case, I think this is something that you should discuss with your cardiologist for the most informed opinion specific to you.
Hope this helps.
Cheers
Bill
Hi, I am a 69 year old male. Never smoked. Avid lifetime runner with approximately 50,000 miles of running under my belt. I had a heart attack two years ago (two 99% blockages of the LAD. Had two overlapping stents of blocked areas.). I’m bike riding now and usually ride 20-30 miles per ride three times a week and average 78% of the age calculated MaxHR for a 65 year old or, specifically, averaging 122 BPM for 1 hour and 45 minutes to 2 hours and thirty minutes. I want to push harder. Am I doing too much? Cardiologist says to do what I want with out restrictions.
Hi Bill
Thanks for your comment. It’s hard to say what’s necessarily “too much” because it really depends on the individual. To your credit, being an athlete your entire life and being more in tune with your body, you’ll have a better gauge on your exertion level, as opposed to someone who’s been relatively inactive their entire lives.
The most important thing is that you are not having any signs or symptoms while exercising. If you are able to sustain your target heart rate over the course of 20 to 30 miles, then I’d say that doesn’t sound like an unreasonable heart rate.
Also important is that your cardiologist has given you clearance to exercise (assuming everything is working well and there are no hidden surprises). Usually during an angiogram, the doctor will have a look at other arteries to get a gauge on things. So assuming your other arteries are clear and you are NOT symptomatic in any way then, realistically, you’ll more than likely be fine.
In order to work to the higher workloads, just be careful and try to systematically push up your intensity in tiny increments. This will allow your body to adapt naturally and also remove the risk of really going all-out, full-throttle. Provided you’re increasing your workload slowly and gradually over time, you are minimising your risk.
Hope this helps.
Kind regards,
Bill
I am 74 yrs old and had a heart attack 12 weeks ago with 100%blockage in a right artery.
Prior, I had been running and going to the gym 5-6 days a week, am not overweight, don’t smoke, and never had a noticeable symptom.
I have gotten back to running and weights with Dr ok, but am unsure at what is to much or too little. I have run up to 3.5 miles and lift various weights at the gym.
Any guidance or perspective is appreciated. Thank you.
Roger
Hi Roger,
Thanks for your comment. The good news is that you were previously active and did not have a lot of risk factors to begin with. If you’re now 12 weeks post-op and are not having any signs or symptoms while exercising, AND you also have clearance from your doctor, then those are good reassurances that you should be able to tolerate higher workloads. You didn’t mention whether or not you’ve had an angioplasty with a stent, but assuming they reopened the artery and the stent is working well, then this will certainly give you a confidence boost.
Also, it may be worth asking your doc if there was any damage to your heart muscle. Not all heart attacks result in cardiac tissue death if you receive treatment in a timely manner. You could have had what’s known as “stunned myocardium” and this can regain its contractile properties over time.
If you can find out your ejection fraction, that will also give you an idea of how well your left ventricle is functioning. So if you’re anything above 50% or so, then you should be ok to do most exercises. Given that you’re already active, then I would think you’re probably up in the 60%s, give or take.
So assuming you’ve had treatment (angioplasty/stent), your cardiac muscle is normal, and your ejection fraction is normal, then you should feel confident to be able to return to most of your pre-heart attack exercises. Of course it’s important to still monitor yourself for any signs or symptoms along the way and, if anything feels out of sorts, then go see your doc for further work-up. Hope this helps!
Cheers,
Bill
Hello Dr,
Came across your webpage and felt very nice going through your encouraging words for the patients.
My husband aged 49, suffered a heart attack about 4 months ago in spite of regular exercise, healthy weight, healthy food habits.
He underwent stenting and was diagnosed with triple artery disease during angiogram. He had 100% block in one of the artery and about 40% and 60% in the other two.
So he was discharged on all the regular medications. Since there are no cardiac rehab programmes in India after such incidences, my big concern is how much to exercise. Right now, he has started slowly with swimming lesson and walking and stairs.
His EF was 43% immediately after stenting and 72% after 3 months of recovery. He was mildly hypertensive before heart attack.
My question is:
Will exercise accelerate blockage?
Is CT angio necessary every year?
What should be his maximum Heart Rate while exercising?
It will be very kind of you if you can advice on the above topics.
Thank you in advance.
Concerned wife.
Hi Ramya,
Thanks for your comment. I’m sorry to hear about your husband having to go through all this. It’s overwhelming when it all lands on your lap at once. But the good news is that he received proper treatment and his ejection fraction at 72% is quite good. If there was no damage to his heart muscle then this is also very reassuring in terms of his ability to exercise.
In response to your questions:
1) No, exercise will not accelerate the blockages. In fact, the opposite is true. People who have had a heart attack that exercise actually have a lower risk of having a second heart attack. Exercise is protective. Exercise “can” be a risk if the person is high risk for a heart attack and has not had an evaluation and treatment by a cardiologist. But in your husband’s case, at least they caught it in time and now it’s a known issue that has been stabilised. So exercise from here on out SHOULD be included in his daily routine.
2) It’s unlikely your cardiologist will do an angiogram every year unless your husband is symptomatic. Remember that an angiogram is still a surgical procedure and any surgical procedure can carry risks. So unless there is a pressing reason to do the angiogram, I would say this is unlikely to be a yearly thing. The doc might opt for a yearly treadmill stress test to see if there are any abnormalities on the ECG. If there are any abnormalities, THEN they might consider another angiogram.
3) Regarding max heart rate while exercising, it’s hard to say because everyone’s heart is wired differently AND may be on medications such as beta blockers that will lower heart rate at rest and during exercise. So using a 1 to 10 scale, have your husband judge his exertion level. 1 would be at rest and no effort at all. 10 would be maximum and completely exhausted. 5 would be sort of middle of the road comfortable level where he can continue the exercise for a while without any heavy fatigue. A 6-7 would be where he is breathing a little heavier but probably could not continue it for hours and hours.
Once your husband locates an effort level of around 6 to 7, he should take his pulse and write down the number. Then when he’s exercising the next time, he can see if his heart rate is around the same at the same effort level of 6 to 7. It takes time to sort of “tune in” to the scale but once he gets used to it, he can cross reference his heart rate with the effort level scale.
The good news is that over time, his heart rate will probably continue to lower with regular exercise. This is a normal adaptation and it means that when he gets to a 6 to 7 on the effort level scale, he will likely be able to sustain a higher heart rate for the same effort. In other words, he is getting more fit as he adapts to exercise again.
Hope this helps.
Kind regards,
Bill
I(30years old 95kg) decided to take magic truffles to remove the stress from my life.After doing some research I decided trying approx. 8 grams of fresh truffles from a legal shop in Amsterdam.Same day before chewing truffles around 2 hours before, I have eaten 2 brownies that contain cannabis from a coffee shop in Amsterdam.
My experience after chewing truffles was really awful and had very bad trip. After 5 hours I returned to normal . This will be my one and only time using this. However even 2 days passed since I returned to normal;I still feel a mild pain in my heart and beating. I went to home doctor and she said my heart is beating normal and my blood values are normal. The mild pain and beat in my heart will end soon? or truffles damaged my heart? I am sceptical. I would be happy having your say in my situation and of course if you have any recommendation
Hi Simon,
It looks like you mixed a lot of things in a short period of time. And while magic truffles and cannabis can be safely consumed in moderation, if your dose was a bit higher and you mixed psychedelic mushrooms with cannabis, then that could very well induce some scary side effects. While I can’t tell you what to do, just remember, as with anything, the devil is always in the dose. Stay safe!